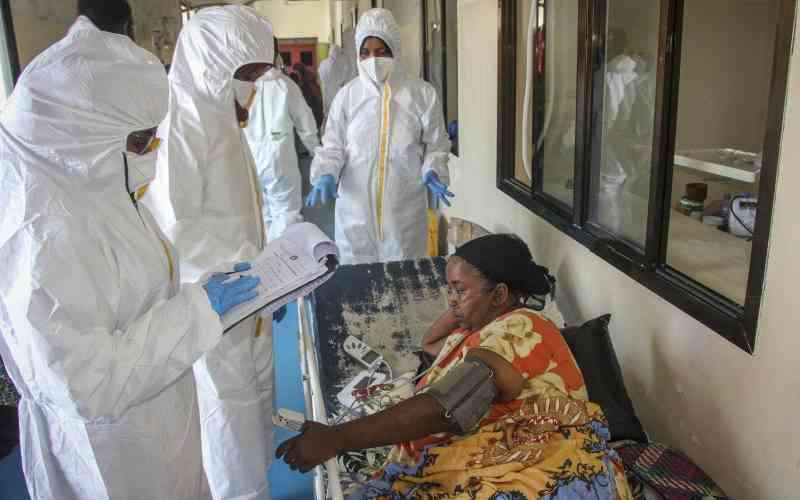
The Covid-19 pandemic devastated the African continent in many ways economically, socially, and politically with the disruptions evident in all parts of the world.
However, like other pandemics and epidemics, Covid-19 has exposed critical failures in multilateralism and global solidarity. Africa has remained among the last in line to access necessary medical supplies and tools - from personal protective equipment to diagnostics, therapeutics and vaccines.
African local manufacturers are at a competitive disadvantage due to the different market forces including poor and inefficient production value chains, high cost of production of medicines and vaccines, poor financing, and financing models and hence important to open and sustain the financing discussions to raise funds specifically for African manufacturing.
In response to the systemic failures in global health security architecture, Africa has witnessed remarkable regional and national leadership in responding to the pandemic and importantly, in identifying what needs to be done and prioritised in the quest to strengthen both national and continental health security.
The Second International Conference on Public Health in Africa (CPHIA) - convened by Africa Centers for Disease Control and Prevention (Africa CDC) in December 2022 presented a platform for different stakeholders to share lessons and outline what needs to be prioritised to strengthen health security in the continent. The underlying consensus at a side event co-convened by the Coalition for Health Research and Development, South African Health Technologies Advocacy Coalition and Pandemic Action Network at CPHIA 2022 was that - only a strong and sustainable local manufacturing industry will strengthen global health security and afford Africa a robust system that would sustainably increase access to life-saving health products and reduce reliance on other regions, when pandemics and other health crises strike.
Other platforms
It is easy to forecast this as an important agenda in other conversations this year including in the upcoming Africa Union Summit in February 2023, the Africa Health Agenda International Conference 2023 in March and the World Health Assembly in May 2023, among other platforms.
As the political leaders, private sector, academia and civil society actors increasingly show convergence on what needs to be done to enhance health security in the continent from what they speak, it is time to accelerate the action. The continent must not be found unprepared and without resilient health systems when the next pandemic strikes. Some key recommendations from the discussions in Kigali point to the areas requiring accelerated action. Firstly, Africa governments play a central role in sustainable financing and institutionalization of a streamlined regulatory system that encourages research and development, domestic product development and sustainable incentivization of the private sector.
- From Monkey pox, Covid-19 and Nipah virus: Why animal-to-human diseases are on the rise
- From wagging tails to healthy tales: How pets improve mind and body
- Why US is experiencing largest measles outbreak
- State: Covid-19 variant in US 'not alarming'
Keep Reading
Intensive efforts
These efforts will contribute immensely in not only attracting investors, but also pool expertise and capacities in and across countries, sectors to enhance coordination in the development of high-quality local products that reach the people who need them.
It is imperative to fast-track operationalisation of the Africa Medicines Agency - a continent-wide platform for strengthening and harmonising continental and regional regulatory authorities. With barely half of the 54-member states having ratified the AMA treaty, it is critical that other member states expedite the ratification of this treaty.
The focus must also be on addressing the issues of cost and access to medical products for citizens. African governments must demonstrate commitment to purchase African-made products - an initiative that will require policy and legislative reforms at country level.
Secondly, African governments must nurture partnerships that seek to prioritize technology co-creation rather than technology transfer. Co-creation of technology will sustain a viable ecosystem that incorporates the needs and priorities of the target population from the onset. It will also open doors to a more sustainable and equitable process that is mutually beneficial for African countries and international partners.
Nevertheless, Africa's first mRNA technology and transfer hub, based in South Africa, is a promising initiative that should be supported, as it has the potential to transform medical countermeasure innovation, particularly for vaccine production.
Finally, there is need to build strong coordination mechanisms across the manufacturing ecosystem with clear cut frameworks that leverage private sector engagement and cross-sectoral collaboration. Commercial viability is not an incentive and most would be investors would shy off from investing in a public good that does not add to their shareholder value.
Industry needs
By working together, we can better understand the industry needs - from infrastructure and staffing to business plans and profit margins.
To this end, concerted efforts and a collaboration of the civil society and non-governmental organizations, governments and multilateral organisations, the private sectors and different investors is key to enshrining public good investments that are alive to needs of the society and the commercial viability resource intensive business enterprises.
The African Union and the Africa CDC's Partnerships for African Vaccine Manufacturing Framework for Action offers a blueprint on how to accelerate local manufacturing in a co-ordinated way. More in-country resources and an enabling environment will provide a domino effect that will guarantee returns in the long run and incentivize governments to facilitate the institutionalization of frameworks that would focus more on the public good rather than government bureaucracy and tax obligations. Partnerships between African countries through joint ventures and centre's of excellence supported by knowledge exchange, capacity building and legislative frameworks would guarantee both opportunities for establishing solid export bases and the possibility of consolidating pharma industries.
Compiled by Dr Githinji Gitahi, Aggrey Aluso, Dr Margareth Ndomondo-Sigonda, Prof Geoffrey Setswe and Dr Simon Agwale
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.











