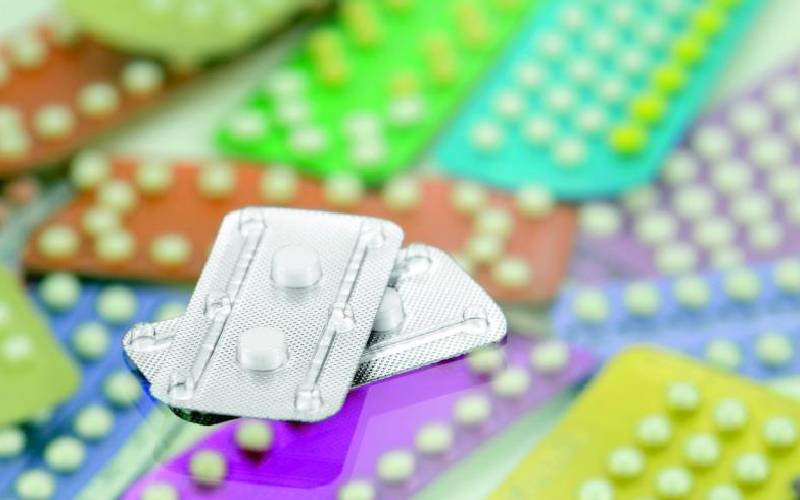
Health experts have raised the alarm over a rapid decline in contraceptive uptake and warned of adverse negative implications in the near future.
Sources at the National Aids and STIs Control Programme indicated that a number of counties had run short of Depo-Provera and implants.
Majority of women are now going for over the counter contraceptives.
In Kisumu, reports from the Department of Health and Sanitation indicated that in August last year, the uptake was at 60 per cent but has now dropped to 40 per cent.
According to the statistics, Kisumu central has recorded a decline of 73 per cent while Seme has dropped from 64 per cent to 40 per cent.
In Nyakach sub-county, the use of contraceptives now stands at 28 per cent, a drop from 38 per cent, with the other four sub-counties recording an average of 20 per cent drop.
The development is a major setback to the health sector that has been running a family planning campaign in the region. Projections show if the trend continues, use of contraceptives will further drop by another 20 per cent in the next four months.
The county’s Reproductive Health Coordinator Jane Owuor said there was a correlation between the sudden drop in uptake of contraceptives to Covid-19. She explained that shortly after coronavirus was detected in the country, public health facilities had run out of contraceptive choices.
“There was a hitch, but currently we are trying to ensure clients access contraceptive choices,” Ms Owuor noted.
Constrained funding
The decline is also attributed to poor health infrastructure and constrained healthcare funding, as the county lacks specific budget for family planning.
“Recurrent strikes by health care workers and inadequately skilled workforce to provide quality family planning services have been attributed to the drop,” she said. Owuor also linked the drop to irregular supply of contraceptives and relevant equipment.
Leah Okiri, a gynecologist at Jaramogi Odinga Oginga Teaching and Referral Hospital, attributed the situation to women shying away from hospitals for fear of contracting Covid-19.
Statistics at the facility indicate that only five clients, from an average of 20 before Covid-19, visit in a day.
“We may not see the impact now, but later it will be felt because there is a possibility of increased family size,” noted Dr Okiri. With an increase in family size, the experts project rise in the poverty index in the region.
“There has been a fear about clients coming to the hospital and this will have negative implications in the future,” she said.
Dr Okiri noted that during this pandemic the clinic has remained open to anyone who wishes to seek family planning services.
However, Kisumu Medical and Education Trust CEO Monica Ogutu said shortage of key family planning choices had seen women stop seeking the services.
“Many women visit hospitals and when they miss out on their choice of contraceptives, they don’t return nor accept alternatives available,” Ms Ogutu said.
She wants the county to prioritise family planning and mobilise resources to ensure sustainability of the family planning campaign. She observed that financing for reproductive health had been shrinking, as a big fraction of it was always from donor funding.
County Health Executive Boaz Nyunya said Covid-19 had disrupted essential service delivery. He noted that there was a drop in aspects of essential services, including antenatal care, deliveries and family planning services. “Healthcare workers must be reorganised to be able to provide essential services. No service should be crippled in the process of responding to Covid-19,” he said.
Last week, Kisumu County officials unveiled a Family Planning Costed Implementation plan 2019-2023, which is meant to increase access to reproductive health services, including maternal and neonatal.
Currently, county antenatal coverage stands at 80 per cent, with skilled birth attendants at 66 per cent. Maternal mortality has been on the rise at 194 per 100,000 live births, excluding community maternal deaths.
Neonatal mortality rate is at 11 per 1,000 live births. The county has prioritised Universal Health Care (UHC) to help lower the neonatal and maternal death.
Last week, Kisumu county government signed a memorandum of understanding with NHIF, which will see UHC services provided to 45,000 households who cannot afford medical care. The projects starts from October 1. “When we meet family planning needs, we will reduce maternal and infant mortality and prevent unsafe abortions, which take place in back streets dens,” Nyunya said.
He added that unplanned pregnancies reamined a challenge in Kisumu, with officials grappling to debunk myths and misconceptions surrounding family planning.
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.