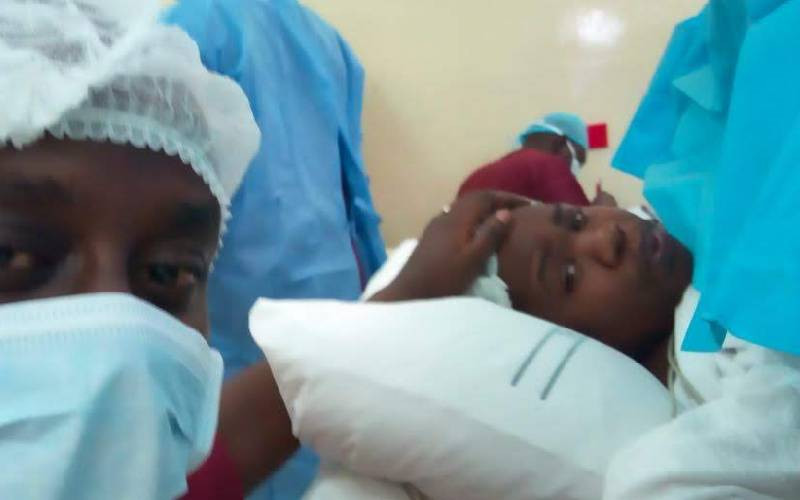
Jacqueline Jude with her daughter Zawadi. [Jonah Onyango, Standard]
She peed in a cup at the health centre, praying that the chemotherapy was not bringing up other health problems. She had walked into the facility after feeling worse than usual. Chemotherapy effects were bad, but this morning she felt worse. She just wanted to be fine, then she would finally start enjoying her new marriage.
A few moments later, the young medical officer walked up to her with a smile. “You have nothing to worry about. You are pregnant,” he said calmly. Jackline Kanyua was not sure how to feel about the news. On one hand she was happy, motherhood did not seem like a far-fetched dream anymore.
Facts First
This story continues on The Standard INSiDER. Subscribe now for unfiltered journalism that holds power to account.
Already have an account? Login
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.