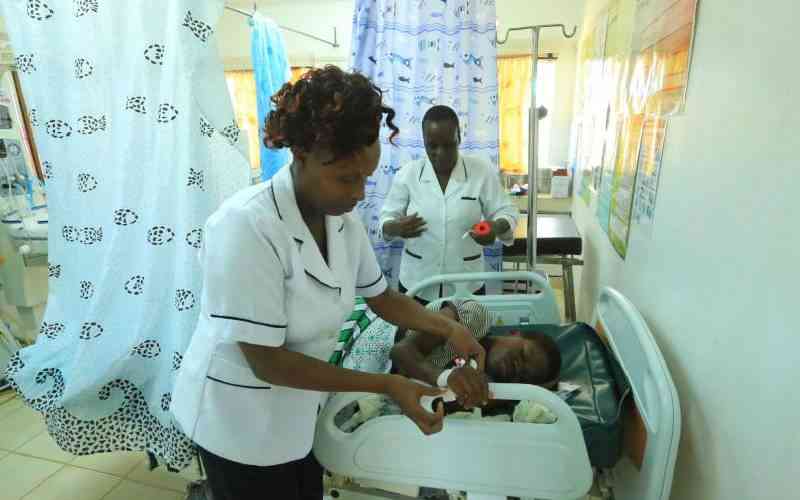
80 percent of hospitalized Covid-19 patients receive prophylactic antibiotics, which could lead to a rise in drug-resistant infections. [Courtesy]
You are a health care worker dealing with the uncertainties of effective treatment protocols early in the pandemic. You prescribe antibiotics for a patient with Covid-19 to treat a possible co-infection or secondary infection; although you’re not sure that they have one.
Now, assume you’re a daily wage worker in a low- or middle-income country with flu-like symptoms. Worried about missing work, you go to a local pharmacist who prescribes antibiotics without considering the possibility of a viral infection such as Covid-19 that does not require such drugs.
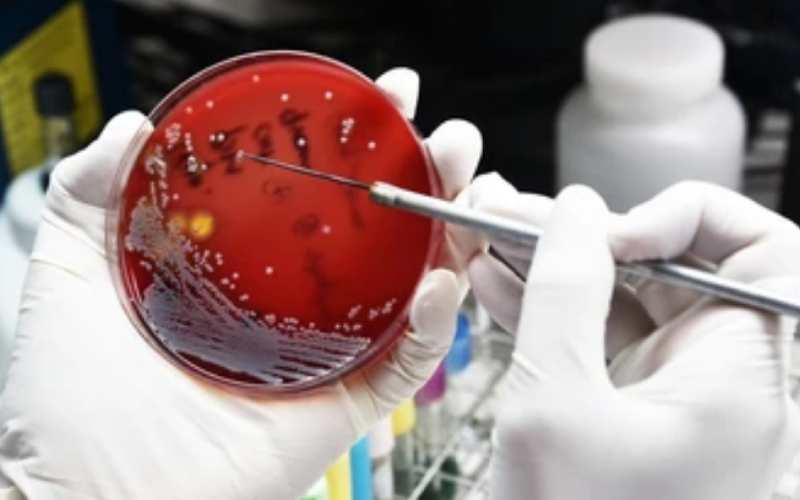
Both scenarios illustrate how antibiotic resistance, already a severe problem, has grown worse in the era of Covid-19.
Recent studies have shown worrying overuse of antibiotics while treating Covid-19 patients, despite low co-infection rates.
Globally, about 80 percent of hospitalized Covid-19 patients receive prophylactic antibiotics, which could lead to a rise in drug-resistant infections. And in places like Lebanon, Covid-19 has contributed to a rollback of antibiotic regulations, making it once again possible to access a wide range of antibiotics without prescription.
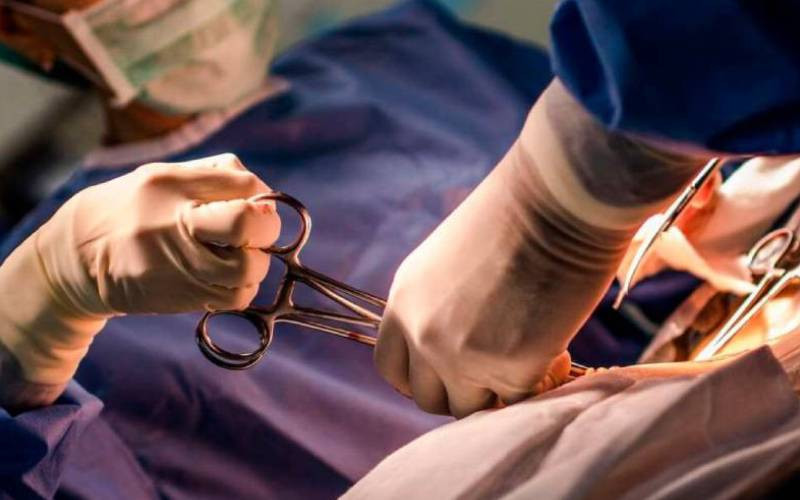
A second, silent pandemic is spreading before our eyes as more bacteria are becoming resistant to antibiotics. If we continue down the current path, routine procedures like a Caesarean operation or a joint replacement will one day become be too risky to perform. The lives of cancer patients and others who undergo treatments that depress the immune system will equally be threatened.
This indiscriminate use of antibiotics for Covid-19 patients could lead to millions of deaths most likely in Low and Middle-Income Countries (LMICs) particularly in Asia and Africa. Countries such as Kenya have recommended the use of antibiotics only in the case of severe acute respiratory illness in their Covid-19 treatment guidelines. However, since most of these treatments can be accessed without a prescription, they are prone to misuse even for those with mild disease.
We can stop the spread of resistance by re-establishing or strengthening anti-biotic stewardship programs to prevent misuse and overuse and to ensure antibiotics are taken responsibly to effectively treat bacterial infections.
LMICs especially face special challenges. They tend to have both unregulated access (which leads to the overuse of antibiotics, and thus antibiotic resistance) and limited access (which leads to death by infections that might be treated by antibiotics).
The latter is the most immediate problem, since lack of access to antibiotics in LMICs is estimated to cause eight times more deaths annually than those caused by drug-resistant infections (5.7 million versus 700,000). However, in the long run, both issues must be addressed.
Several groups are working to ensure better access to quality antibiotics and counter antibiotic resistance. For example, CARB-X, the global non-profit partnership Combating Antibiotic-Resistant Bacteria Biopharmaceutical Accelerator, aims to accelerate antibacterial research to combat the rising threat of drug-resistant bacteria.
By pooling funding, it plans to bring better antibiotics to more patients by 2030. GARDP, the (Global Antibiotic Research and Development Partnership), aims to develop five new treatments by 2025 to fight some of the most threatening drug-resistant infections.
Real lives are at stake. Consider: More than 214,000 newborn babies, most of them from LMICs, die each year from drug-resistant infections.
Though the prospects for new treatment bring hope, effective stewardship cannot wait.
An institution, with little or no funding, can take effective steps such as having volunteers carry out awareness campaigns. A dedicated nonprofit might offer health care workers free access to online modules that foster appropriate distribution and use of antibiotics. Policymakers and health officials also have a role, for example, by helping increase access to high-quality rapid diagnostics tools, which confirm whether antibiotics are necessary - and so preempt superfluous use.
Antibiotic resistance is a problem that affects us all. Likewise, new treatments will benefit us all. But without appropriate safeguards in place, research into new antibiotics will be wasted.
Like Covid-19, the silent pandemic of antibiotic resistance requires global solutions so that all infections are treatable for everyone, everywhere.
Manica Balasegaram, is Executive Director, Global Antibiotic Research & Development Partnership.
Dr Monique Wasunna,is the Director, Drugs for Neglected Diseases initiative, Africa regional Office
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.