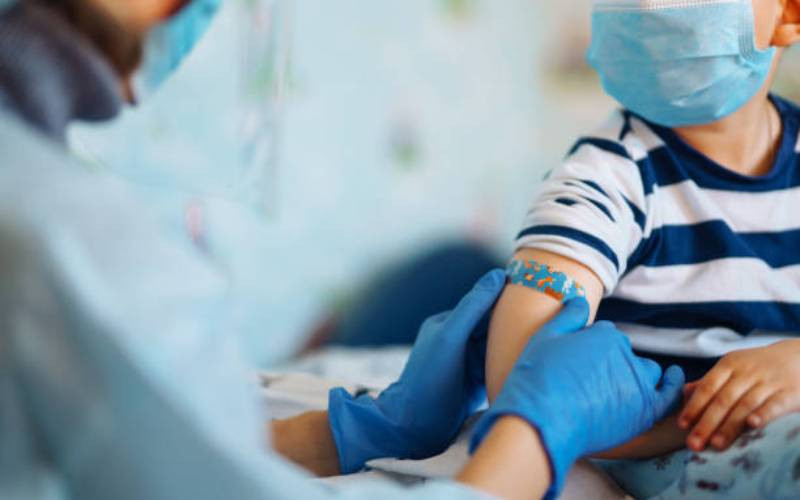
About six out of 10 children get jaundice when they are born. This usually harmless condition - seen two to four days after birth - is characterised by a yellow appearance of the eyes and skin. Ideally, it should disappear within the first three weeks but if not resolved by then, there could be underlying conditions contributing to it.
These include:
Facts First
Unlock bold, fearless reporting, exclusive stories, investigations, and in-depth analysis with The Standard INSiDER subscription.
Already have an account? Login
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.