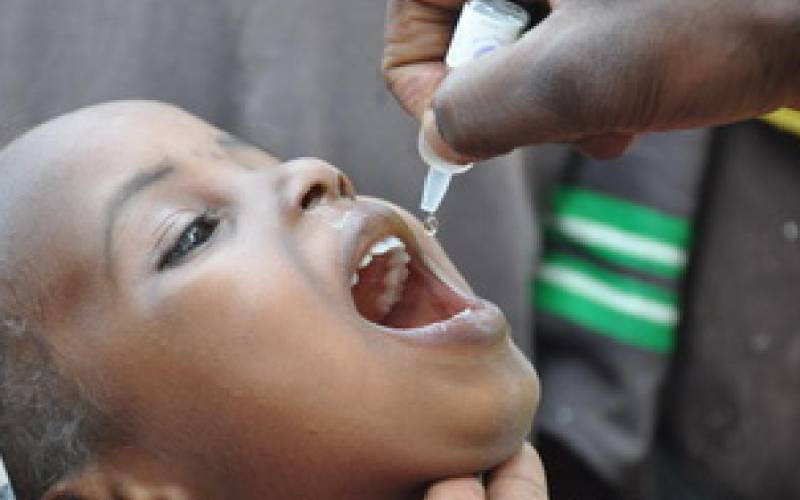
As Kenya joined the rest of the world to celebrate World Malaria Day yesterday, the county has directed that all patients seeking treatment for malaria be tested for Covid-19.
This comes even as counties are grappling with shortage of testing kits, paralysing contact tracing and surveillance aimed at breaking the chain of transmission of the virus.
Malaria positivity rate in Trans Nzoia stands at 21. 99 per cent, against Covid-19 positivity rate of 13.4 per cent.
By Friday, the county had recorded 1,139 cumulative Covid-19 cases since the pandemic was reported in the country in March last year.
Patients exhibited symptoms such as fever, joint pains, muscle pains, loss of appetite and general body weakness.
County Health Executive Clare Wanyama said the symptoms were overlapping in both diseases, and therefore during the pandemic, there should be high index of suspicion.
“Malaria is endemic disease in the region and because of increased numbers among those testing positive for the virus, Covid-19 is mandatory to avoid spreading the disease at community level,” said Wanyama.
She said the county is using Prevention, Retention and Contingency (PRC) and rapid antigen testing.
However, due to the high number of tests performed daily, the PRC machine requires regular maintenance and repair. It is currently not functioning.
Samples collected through target testing are taken to Moi Teaching and Referral Hospital (MTRH) or Kenya Medical Research Institute (Kemri) in Kisumu for tests.
“Hospitals are currently depending on antigens but we have acute shortage of testing kits,” said Wanyama.
She said introduction of antigen testing is among measures aimed at boosting the fight against coronavirus.
Antigen testing is a rapid diagnostic test that directly detects the presence or absence of specific protein (antigen) from the virus that causes Covid-19. The technology does not require laboratory for processing and results are released after 15 minutes.
Also, with the technology, individuals who are at the greatest risk of contracting the virus can easily be identified.
“Due to shortage of testing kits, we are conducting target testing. We would, however, wish to have massive tests in the fight against Covid-19, to break the chain of transmission,” she added.
Malaria patients, however, are often shocked and reluctant when directed to undertake Covid-19 tests
Jane Nasimiyu and her three-year-old grandson, were diagnosed with malaria at Endebes Sub-county hospital. They were tested for Covid after experiencing headache, fever, vomiting and fatigue. Their samples were taken to the Moi Teaching & Referral Hospital (MTRH).
“Though I have recovered from malaria, I was taken through Covid-19 tests yet results seems to take longer,” said the 58-year-old, adding that her grandson had admitted for the second time in a two weeks.
“My grandson’s immune system seems to be low. He recovers after treatment but present the same symptoms,” said Nasimiyu. “I am hopeful he will be treated and recover.”
The grandson was among tens of children at the facility’s pediatrics ward where majority of patients had fever and headache.
Nasimiyu hails from Cheptandan village where an upsurge in malaria cases has been reported.
Another patient, Jacob Maina, has been suffering from malaria for the past three weeks.
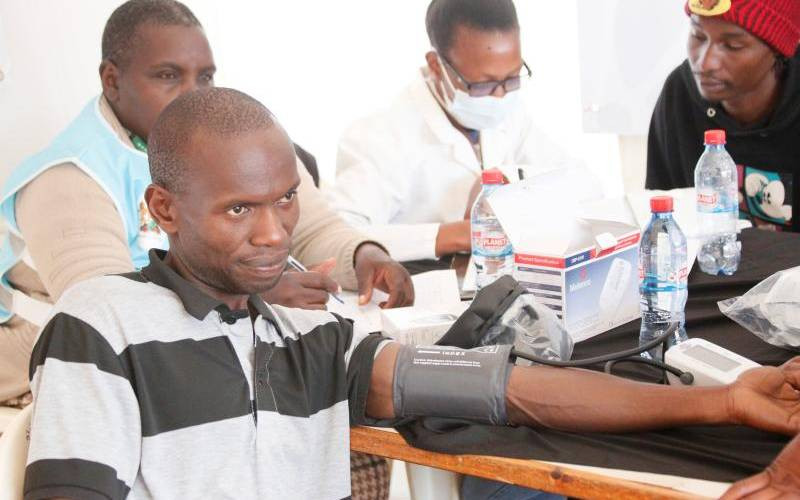
“I was diagnosed with malaria but I still have severe headache and fever. Doctors have advised Covid-19 tests. If I am found positive, I will courageously battle, and if negative, I will be keen,” he said at Bidii health centre in Kwanza area where he was seeking treatment.
The number of patients with malaria-related symptoms at Kitale Referral Hospital is also on the rise with the pediatric ward with a capacity of about 20 children full to capacity.
“The facility is overwhelmed by admissions,” said a clinician. “Most patients who have malaria are children below five years.”
According to World Health Organisation, Covid-19 symptoms include cough, shortness of breath, fatigue, muscle pain, chills and headache.
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.