Kenya is reporting a high burden of curable sexually transmitted infections, a study by the Kenya Medical Research Institution (Kemri) has revealed.
Chlamydia is the leading sexually transmitted disease currently observed in the general population.
Up to one in every five women of reproductive age who are at substantial risk of acquiring HIV have the sexually transmitted disease.
Felix Mogaka, a clinical research scientist at KEMRI - Research Care and Training Programme (KEMRI-RCTP) in Kisumu said the frequency of chlamydia surpasses that of syphilis and gonorrhoea, a trend that is worrying.
"Condomless sex contributes to chlamydia, an infection that may end up making our population face serious consequences, including infertility," said Dr Mogaka.
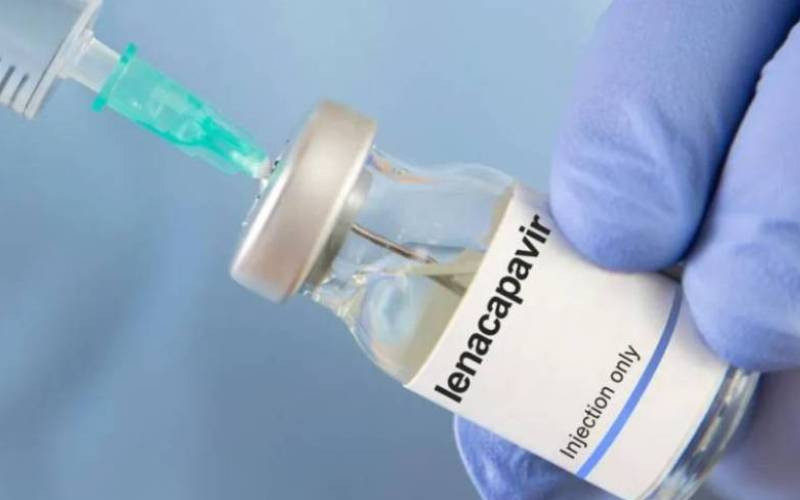
In a study conducted in Kisumu, it was revealed that curable sexually transmitted infections are common among individuals who are on HIV Pre-exposure prophylaxis (PrEP).
HIV PrEP is an antiretroviral medication used by HIV-negative people at substantial risk of HIV, which reduces the risk of HIV acquisition.
"People use Prep to prevent HIV, but unfortunately, it does not prevent against other STIs such as chlamydia can cause complications such as pelvic inflammatory disease, chronic abdominal pain, pregnancy complications and infertility" Dr Mogaka explained, during the Maisha conference in Mombasa.
- Fighting in silence: The untold stories of learners and teachers living with HIV
- Kenya records increase in new HIV infections
- Over 8,500 Nakuru teens infected with HIV in one year
- Alarm as HIV infection among teenagers rises in Siaya
Keep Reading
Worryingly, a large percentage of women who have chlamydia and gonorrhoea, representing up to 70 per cent, do not have any symptoms and are therefore unlikely to seek treatment.
The country does not have a programme to do laboratory screening for chlamydia and gonorrhoea and instead depends on making diagnoses based on symptoms, leaving out the large number of women who have an STI but have no symptoms.
Due to a lack of symptoms, most patients present to hospitals at an advanced stage of the disease, according to the researcher.
Doctors rely on symptoms to treat Chlamydia, but it is ironical because, in many women, it does not present with any symptoms. If you rely on symptoms to make a diagnosis, you miss all these people," he said.
He added: "There are more people with chlamydia than people with gonorrhoea and syphilis. Most people do not know about chlamydia because when people hear about STIs, they think about gonorrhoea and syphilis, actually chlamydia is the mostcommon STI."
In the study carried out in Kisumu, the research team noted that women had high rates of bacterial STIs namely chlamydia trachomatis, Neisseria gonorrhoea, and Treponema pallidum.
The primary objective of the study was to evaluate whether doxycycline, an inexpensive and commonly available antibiotic, would prevent STIs among women using PrEP when used for prevention rather than treatment.
In the study, the participants took doxycycline within 72 hours of having condomless sex.
In previous studies among men and transgender women taking HIV PrEP with high rates of STIs, doxycycline post-exposure prophylaxis (PEP) significantly reduced incident STIs.
However, there was no data on whether doxycycline is effective in preventing STIs among women on HIV PrEP in Eastern and Southern Africa, who have STI rates similar to or higher than those seen in people using HIV PrEP in the Global North.
The study was first done in Kisumu among women.
At least 449 non-pregnant women aged between 18 and 30 years and taking HIV PrEP participated in the study during the study between 2020 and 2022.
The findings from the study showed that the use of doxycycline post-exposure prophylaxis did not reduce new STI infections among women, a stark contrast to the results from men and transgender, where doxycycline significantly reduced the frequency of new STIs.
Dr Mogaka explained that the lack of effectiveness could be due to the low use of doxycycline post-exposure prophylaxis by the study participants.
When the researchers tested for the presence of doxycycline from some of the samples collected during the study, doxycycline was not detected in 44 per cent of study participants who should have been taking it.
In the presentation, scientists emphasised that the burden of STIs is high among women on PrEP and highlighted the need for STI-preventive options for women that are effective and acceptable.
They noted that adherence to preventive medicines needs to be better understood and supported for biomedical prevention to be effective.
Globally, doctors are using laboratory diagnosis to screen for chlamydia disease in populations with high rates of STIs, which is yet to be adopted in Kenya as it is expensive.
Mogaka said scientists are advocating for the adoption of point-of-care tests to test and treat sexually transmitted diseases.
"For effective control of STIs, we need to adopt technologies whereby someone comes in, and they can be tested and given their results within that consultation and treated.," said the researcher.
In Kenya, he observed that most people go to pharmacists as their first point of contact when they have an issue.
Pharmacists can leverage pharmacies to do testing and treatment. We need to spread the services out so that they can be accessed by everybody- pharmacies, family planning clinics, antenatal clinics, STI treatment clinics," said Dr Mogaka.
Common STIS within the Kenyan population according to data by the ministry include gonorrhoea, syphilis, and mycoplasma genitalium.
There are also, other sexually transmitted infections, including bacteria Trichomonas vaginalis trichomoniasis and Vulvovaginal candidiasis that are also common among this population.
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.