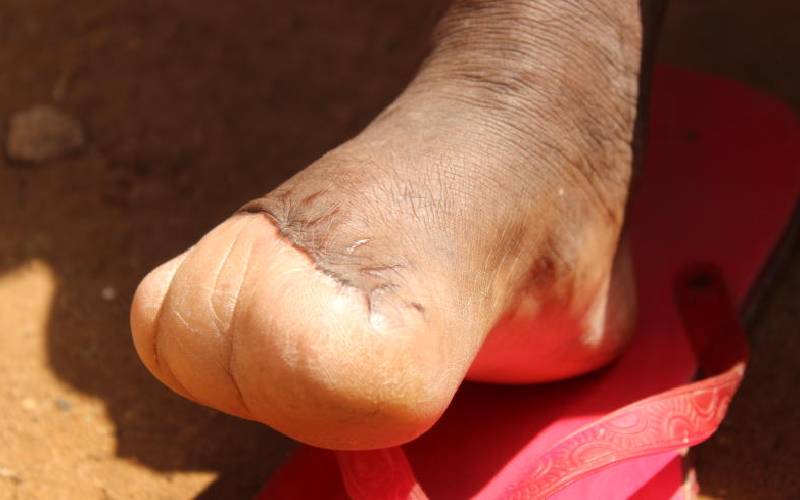
Amputated left toes of Beatrice Ikamba Runji. [Christopher Kipsang, Standard]
Beatrice Ikamba Runji, a house help, felt tired and decided to rest her then 51-year-old body in 2015.
As she removed socks to take a nap on the couch in Kanganangu village, Mbeere sub-County, she felt her right foot caked in blood- she had a prick, the foot was badly hurt and oozing blood.
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.