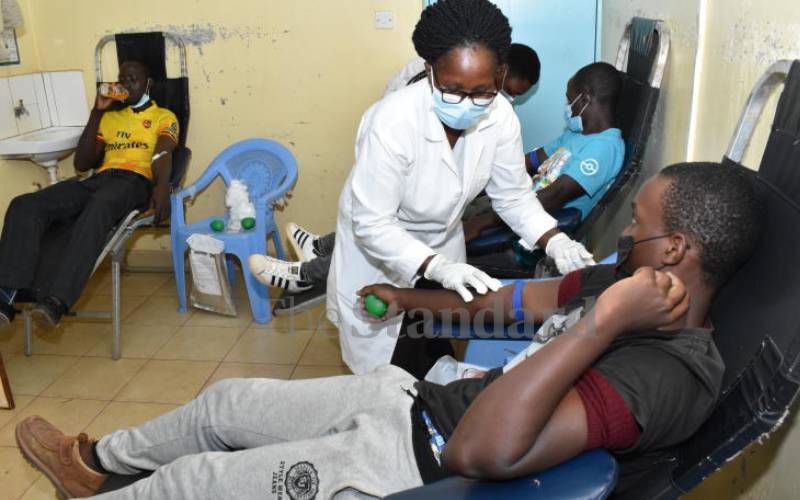
Expectant fathers donating blood at Thika Level Five hospital, March 1, 2022. [Samson Wire, Standard]
Kevin Thiong’o, a resident of Juja, woke up early to accompany his wife for Antenatal care (ANC) at Thika Level Five Hospital.
Being a first-time father, he is anxious.
Facts First
This story continues on The Standard INSiDER. Subscribe now for unfiltered journalism that holds power to account.
Already have an account? Login
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.