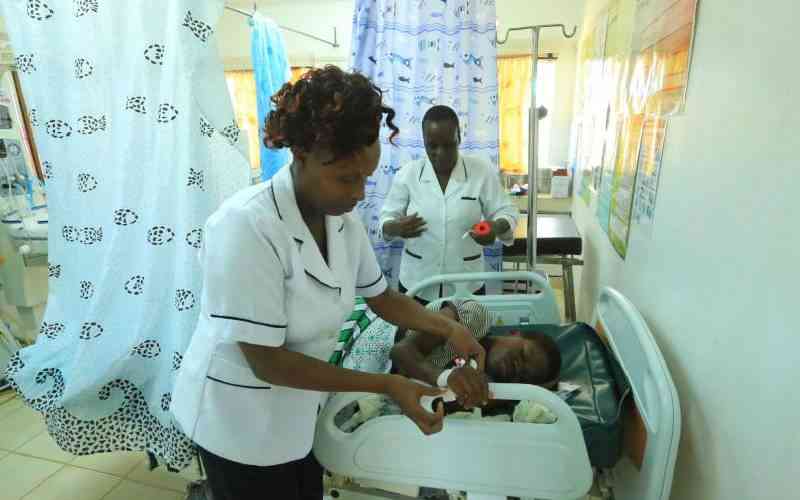
Ruth Wanjogu is weak, and in pain. She lies helplessly at the Rift Valley Provincial General Hospital casualty area hoping to be checked by a doctor.
Wanjogu, 55, left her home at Eburu village in Gilgil at around 4am and arrived at the hospital at 7am. But by 4pm, she is yet to see a doctor.
She has a heart problem, her two limbs have fresh wounds and she uses a walking stick to support herself.
"I have acute headache, and the pain in my limbs is too much," she said.
Prior to the visit, she had been admitted to Ward 8 for five days in January, after she developed the wounds.
She claimed a doctor carried out a test then that revealed she has a heart-related condition, and required quick attention. She was given drugs and asked to come back after a month for check-up.
On several occasions, she has been to the hospital and left without seeing a doctor because of long queues.
Sometimes she stays with well-wishers. She told The Standard team she had carried her bedding and would camp at the hospital until she was examined by a doctor.
Deep pain
"Feel my heart. The heartbeat is so fast and I am in deep pain. I hardly sleep at night," she said.
Gladys Njambi, 75, from Ngashura in Bahati, is also among patients in agony waiting for services at the facility.
Njambi was electrocuted on Saturday, but long queues at the hospital have not allowed her to be attended to. She has acute headache and general body weakness.
"I arrived here at 8am, but I am yet to see the doctor. I fear I might go back home without being examined," she said.
This is the agony patients seeking services at the referral hospital and paints a picture of what many public health facilities are grappling with.
Failure by county governments to guarantee doctors' study leave and alleged harassment from political leaders has seen many doctors under devolved units resign.
In the South Rift, over 100 doctors have resigned in the past two years.
Resignation of both medical officers and consultant doctors, according to Kenya Medical Practitioners, Pharmacists and Dentists Union (KMPDU), has highly affected discharge of health services.
“There is high shortage of doctors serving in public hospitals,” says KMPDU South Rift Secretary General Dr Davji Atellah.
The most hit county in the region is Nakuru where at least 40 doctors have resigned, followed by Laikipia with 34 doctors, Kajiado 13, Kericho 10 and two in Narok.
Ivyn Masinde is among doctors who decided to resign after being denied study leave by Nakuru county government.
Felt stagnated
Masinde had served for three years, and when she felt stagnated, she resigned last September and is currently furthering her studies.
Doctors too are overworked in the county, clocking 168 hours per week instead of 40 hours recommended by world health standards.
In Nakuru, facilities mostly affected include Kabazi, Subukia, Molo, Bahati sub-county hospitals.
In a letter written to Governor Lee Kinyanjui by the union dated January 25, officials want more doctors employed, and the county to address the issue of promotions that have not been effected since 2015.
PGH Medical Superintendent Joseph Mburu admitted there was a shortage of doctors, but said it had not affected service delivery.
“Shortage of doctors is a countrywide crisis in the health sector because some doctors go back to school while others opt to join the private sector,” he said.
There are 25 medical interns employed by the county government at PGH, 15 medical officers and more than 10 specialists and consultants.
At the Rift Valley Provincial General Hospital, there are no radiologists to interpret images.
Dr Mburu is forced to perform administrative roles and also visit the X-ray department to help the nine radiographers there.
Another department that requires more medics at the Level Five facility is the orthopaedic section, because of high number of road accident along Nakuru-Salgaa-Sachangwan stretch.
There are only two orthopaedic doctors and two from Egerton University who conduct operations at the Level Five facility every day.
Contacted for comment, Nakuru Chief Officer of Health Dr Samuel Mwaura said plans to employ more medics are underway.
Greener pastures
He said last year, at least 150 positions for nurses were advertised to fill the gap.
“The county is planning to employ more medics for smooth discharge of health services,” he said.
In the North Rift, tens of doctors and other medical personnel have been resigning to seek greener pastures.
KMPDU cite wanting staff welfare and poor working conditions as the leading causes of mass exit of doctors and other health workers from county hospitals.
Six North Rift counties – Uasin Gishu, Nandi, Elgeyo Marakwet, West Pokot, Trans Nzoia and Turkana – have lost over 24 doctors in the last two years, with a shortage of 105 doctors reported across the counties.
"Each county has a shortage of 15 doctors, with resignations contributing to this situation. We are losing an average of two doctors per county every year," said KMPDU North Rift Secretary General Ishmael Aiyabei.
In Nandi County, five doctors have so far left, throwing the county health services into a crisis.
The situation is no better in Trans Nzoia County where three doctors have resigned to seek greener pastures, while three others left for further studies two years ago.
The county government employed 10 doctors last year.
Similar cases of doctor resignations have been reported in West Pokot and Uasin Gishu counties.
According to the doctors' union, Turkana is the only county in the North Rift that has achieved enhanced service delivery with over 60 doctors currently, with no mass resignations experienced.
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.