This year marks the deadline in which all countries should have met all the Millennium Development Goals (MDG) that the world committed to in 2000. Of the eight goals, Kenya has underachieved in Number Four, reducing child mortality, and Number Five, improving maternal health.
The National Coordinating Agency for Population and Development shows that one in 300 Kenyan women die while giving birth. The country had a target of reducing maternal deaths to 100 in 100,000 births but this has not been achieved.
The United Nations Development Programme (UNDP) MDG 2014 Report lists Kenya among the 25 countries with insufficient progress in curbing the under-five mortality rate.
One of the reasons for this is that most women still give birth at home because they live too far away from hospitals. For this reason, the county governments have invested in emergency response services, including providing ambulance services.
In a recent Infotrak poll, Machakos County was ranked top in providing health services. The county’s administration points to its emergency rescue services as one of the reasons for the good rating.
Governor Alfred Mutua, had on February last year paraded 70 ambulances at the Machakos stadium during the launch of the comprehensive healthcare programme. Besides the ambulance vans, there were ten rapid response motorbikes and 89 security cars.
“In Machakos County, many children are called Nzia, meaning road, because they were born by the roadside... giving birth in Kenya is a precarious affair. Many children are born at home, on the road or in bushes,” said Dr Mutua.
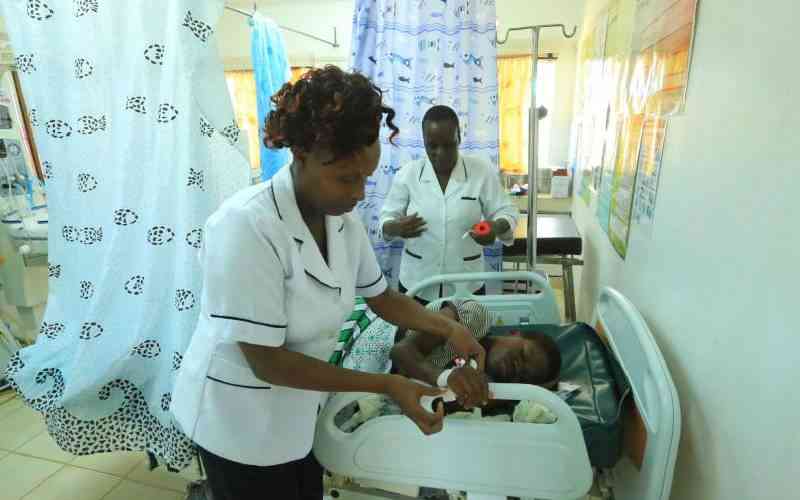
According to a recent Save the Children report, Kenya is rated near the bottom of the best countries to be a mother at 138 out of 179. In many rural areas like Machakos, mothers deliver at home, while others are ferried to hospitals on wheelbarrows and on donkeys.
Exactly a year after the ambulance launch in Machakos, The Standard on Saturday visited the County, to see how the healthcare programme was faring.
“In the one year, I can confidently tell you that no woman has been taken to the hospital on a wheelbarrow...” Mutua told us. “The response time from the patient calling us is very fast, seven to eight minutes.”
At the Control Room, where the security CCTV is manned, we got a glimpse of how the emergency rescue works. The cameras, placed in different areas of Machakos, were broadcasting live images on television monitors.
Kennedy Mutiso, an ICT technician, retrieved one of the archived videos. It showed a lorry at the Makutano junction, which is about 30km from Machakos town. The lorry reversed hitting a streetlight pole.
The pole fell on a man. People milled around the accident scene and five minutes later, an ambulance arrived.
“Watching the accident live from the control room,” explains Felix Musa, the County’s Fleet and Dis- patch manager, “they called an ambulance and sent it to the scene.”
Machakos, unlike most counties, chose to buy ambulances rather than get into partnership with the Kenya Red Cross Society or other service providers.
The hiring has raised a storm in Mandera and Kisii with some arguing that the monthly cost of Sh600,000 for one ambulance is too high.
Two of the counties, Bomet and Garissa, were mentioned in the Ethics and Anti-Corruption Commission list of shame which observed that the costs of hiring ambulances are expensive and exorbitant.
The Director of the Emergency Services, David Mwongela, believes that hiring is costly. He says that Machakos shopped for cheaper vans in China with each costing only Sh1.7 million.
“The vans came equipped with a couch for patients, a trolley, oxygen, a fire extinguisher, radio call equipment, a drip stand and a drugs box,” he says.
All they did was buy the drugs and consumables and hire professional staff. He adds that the vans came with zero mileage, which means they do not need much in terms of maintenance.
“We service them every month at a cost of Sh2,000 each and each year we set aside Sh20 million for fuel.”
This, says the director, leads to efficiency in emergency response and already, “other counties are using us as a benchmark. A few months ago, Kakamega MCAs came to learn from us, and in March all the 47 counties met in Embu to discuss the development of a national ambulance policy. We are the only county with one, and they have been borrowing from us.”
And Machakos County has the numbers to prove that the system is efficient. It has compiled a list of ambulance cases it has responded to which shows delivery complications lead followed by traffic accidents and respiratory disorders.
By December, the county had responded to a total of 9,417 cases. In January alone it responded to 718 cases and 677 in February.
Other counties are emulating Machakos. According to a report by a government agency, the Kenya Red Cross Society (KRCS) signed a memorandum with Garissa County on March 21, last year to provide prehospital emergency medical services in its seven sub-counties.
KRCS is reported to have entered into a similar deal with Bomet on February 10. The KRCS has explained the leasing arrangement it has with its clients.
“We do not just lease out ambulances,” read the press statement from Arnolda Shiundu, the Communications Manager, “but offer a comprehensive service which includes a fully-serviced ambulance, emergency medical equipment and a paramedic in each ambulance.”
In counties like Mandera, there has been a row over whether leasing ambulances is ultimately cost effective.
Mandera governor Ali Roba had hoped that leasing of six ambulances would help in lowering maternal deaths, the highest in the country at 3,795 per 100,000 births.
One of the reasons for the deaths is that hospitals are far apart and can only be accessed through travel on poor roads.
Mandera County Assembly Majority Leader Robow Mohamed Hassan says it is cheaper to hire ambulances as they come with a comprehensive package.
Kisii was among the first counties to get ambulances for pre-hospital emergency medical services on October 22, 2013.
The county’s director of health, Dr Geoffrey Otomu, says that before they got the ambulances, cases of maternal deaths and child mortality were high.
Homa Bay has chosen to buy its own ambulances to cater for emergency cases. It is one of the counties with high rates of maternal deaths and cases of under five children deaths. The county’s maternal mortality stands at 673 deaths per a 100,000 and 170 per 100,000 child mortality rates.
Homa Bay insists that it is doing all it can to reduce the deaths through the provision of emergency services.
Last year, Homa Bay County Governor Cyprian Awiti and his Nyamira counterpart John Nyagarama said they had been approached by service providers to hire ambulances but felt the cost was too high.
Homa Bay County’s Health Executive, Lawrence Oteng says they have fully equipped ambulances to help in health emergency response.
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.