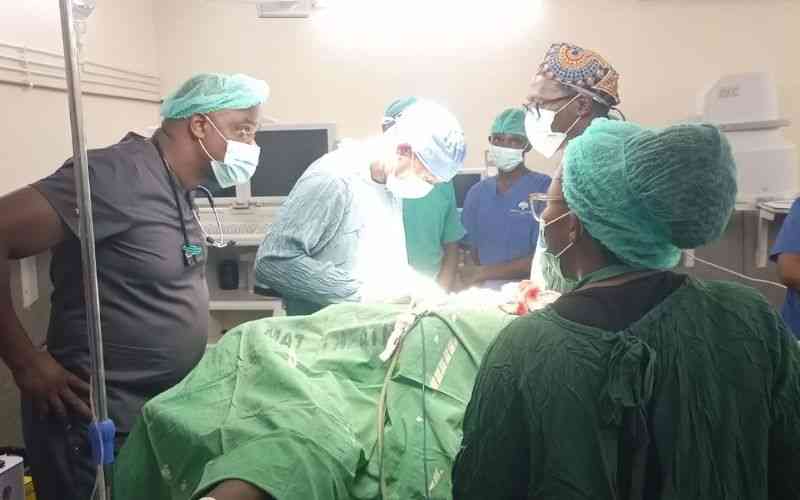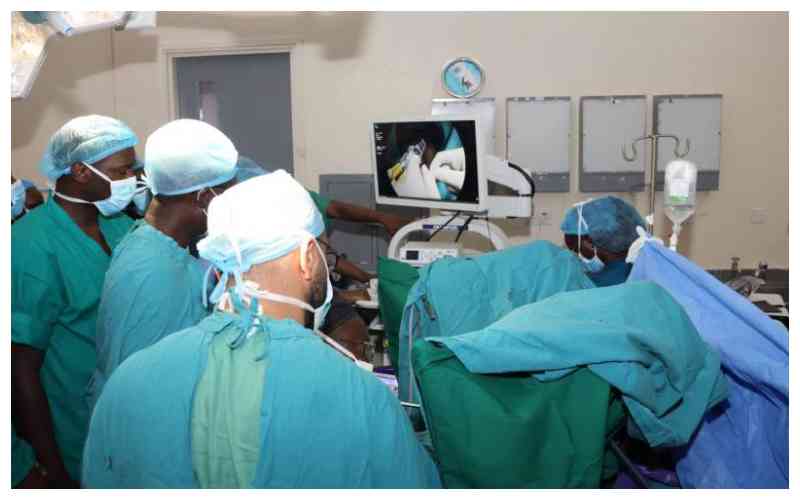
Only 1,426 dentists have been registered by the Kenya Medical Practitioners and Dentists Council since 1978. [Courtesy]
Oral health enables an individual to eat, speak, touch, taste, and convey a range of emotions without active disease, discomfort or discouragement and is an essential component of the general body health.
And the 2015 Kenya National Oral Survey (KNOS), the only such survey so far, sampled five-, 12- and 15-year-olds, and the findings revealed that three out of four suffered from bleeding gums, with a prevalence above 99 per cent in the five-year-olds. Nearly all adults (more than 98 per cent) screened had some form of gum disease.
The study concluded that children and adults had unmet dental caries and gum related treatment needs, with a significant population in Kenya still exposed to fluoride levels above normal in their drinking water.
The oral health-seeking behaviour and oral hygiene practices was found to be poor, with the quality of life adversely affected by existing oral diseases, a situation worsened by the low number of dentists.
Only 1,426 dentists have been registered by the Kenya Medical Practitioners and Dentists Council since 1978. Of these, only 816 are licensed to practice in 2021. Less than half work in public service, meaning we have less than 10 dentists per county or a dentist to population ratio of 1:110,000, according to the 2019 National Census.
Over the last three years, we have seen increased advocacy on integrating oral health into general health, with much attention on non-communicable diseases (NCDs). Oral diseases share modifiable risk factors, with NCDs; cardiovascular disease, diabetes, chronic respiratory disease, cancer and mental and neurological disorders. This means the need for uninterrupted access to oral healthcare cannot be overemphasised.
The importance of this saw the approval of the resolution on oral health at the World Health Assembly (WHA) last May; a landmark resolution that put oral health back on the global health agenda. It formally recognises the need to address oral health as an integral element of the NCD and Universal Health Coverage (UHC) responses.
The resolution also calls for the recommendation to consider ‘noma’ (a flesh-eating infection) as a neglected tropical disease.
This renewed focus means, as a country, we should align our oral healthcare system to focus on these modifiable risk factors-tobacco, harmful use of alcohol and unhealthy diet.
Mouth and throat irritation causes cyclic repair of the soft tissue lining, which is a corollary to mouth and throat cancer. [Courtesy]
The use of tobacco and alcohol has been linked with gum disease, and both are strongly linked with the development of many cancers of the mouth, lips, and tongue- a leading cause of death with a higher preference for the male population.
Recently evidence of health risks due to the use of electronic nicotine delivery systems (ENDS), including e-cigarettes and heated tobacco products (HTPs), has emerged, and research around this continues.
Youth who find it trendy to vape should take caution and know that vape use has been shown to cause mouth and throat irritation, periodontal (gum) damage, and respiratory disease.
Mouth and throat irritation causes cyclic repair of the soft tissue lining, which is a corollary to mouth and throat cancer. Our health professionals, including dentists, have a pivotal role in raising awareness about NCD risk factors among their patients.
However, as a country, we should adopt evidence-based policies to address the root causes of these risk factors, including the social and commercial determinants of health and unhealthy industry interference in policy making.
There is strong evidence of public regulation’s role in reducing the harm caused by unhealthy commodity industries.
There is no known evidence on the effectiveness of industry in self-regulation. Interference by unhealthy commodity industries has been a persistent obstacle to the government developing and implementing NCD policies. Despite the wealth of evidence demonstrating the important role oral health plays in securing general health, oral healthcare is rarely included in countries’ UHC benefit packages. This is the case even in high-income countries.
Yet, studies have shown fewer hospitalisations for at-risk patients who receive integrated medical and oral healthcare services.
The legislative restructuring at the National Health Insurance Fund to convert it to the vehicle for UHC, the elixir for our current situation, has seen it develop a UHC benefits package.
The Kenya Dental Association has proposed dental procedures such as dental fillings, root canal therapy, extractions, full mouth scaling and atraumatic restorative therapies included in the benefits package.
-Dr Tim Theuri is President, Kenya Dental Association and Head of Dental Department, Murang’a County Referral Hospital.
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.