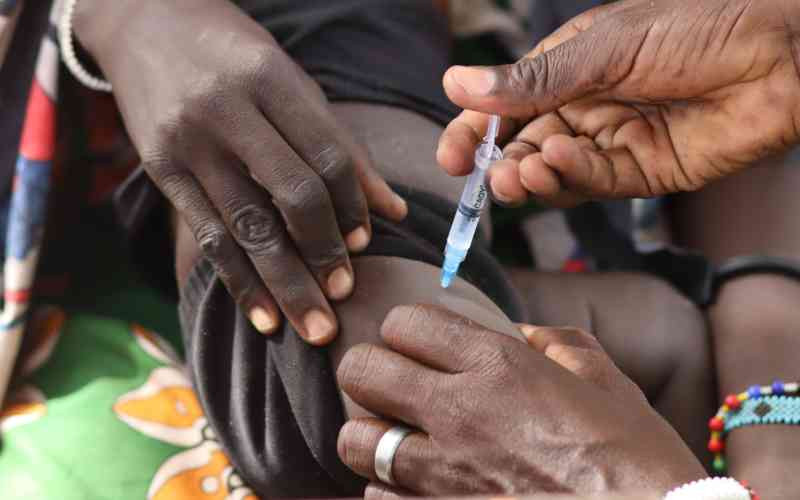
It's 10:46 am and 33-year-old Rachel Simiyu is in deep thought sitting next to her daughter's bed at Bungoma Referral Hospital's pediatric ward.
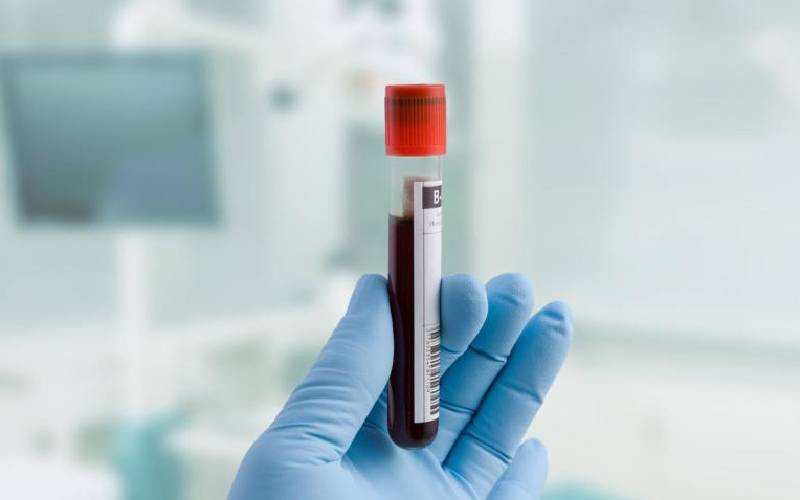
Every 3-4 weeks, Rachel camps at the hospital with her daughter, 11-year-old Michelle, who is battling with a rare but chronic blood disorder.
Facts First
This story continues on The Standard INSiDER. Subscribe now for unfiltered journalism that holds power to account.
Already have an account? Login
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.