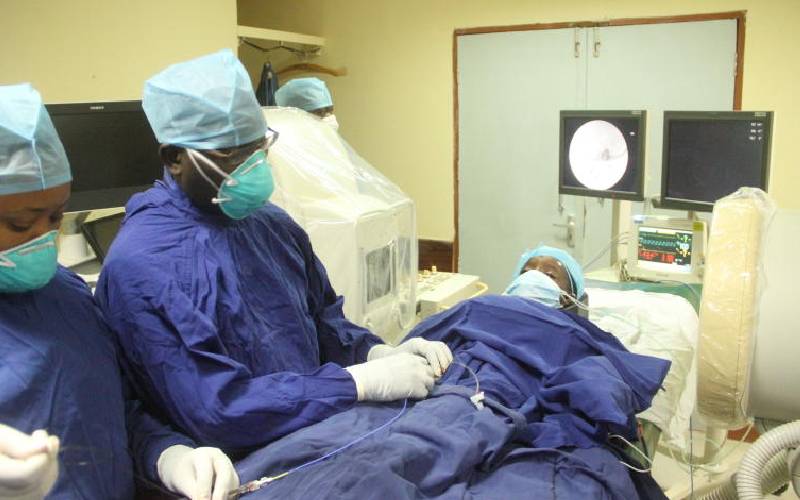
A group of doctors doing internal eye surgery on four years old on March 18, 2021, at Kenyatta National Hospital, in Nairobi.[Edward Kiplimo,Standard]
Seven-year-old Fancy Chepkoech was diagnosed with cancer of the kidney at Rift Valley Provincial General Hospital in 2019. She had the affected kidney removed after the discovery of cancer known as nephroblastoma.
In July last year, the girl again developed sharp abdominal pains. In September, she was referred to Kenyatta National Hospital (KNH) for review and removal of a growth.
Facts First
This story continues on The Standard INSiDER. Subscribe now for unfiltered journalism that holds power to account.
Already have an account? Login
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.











