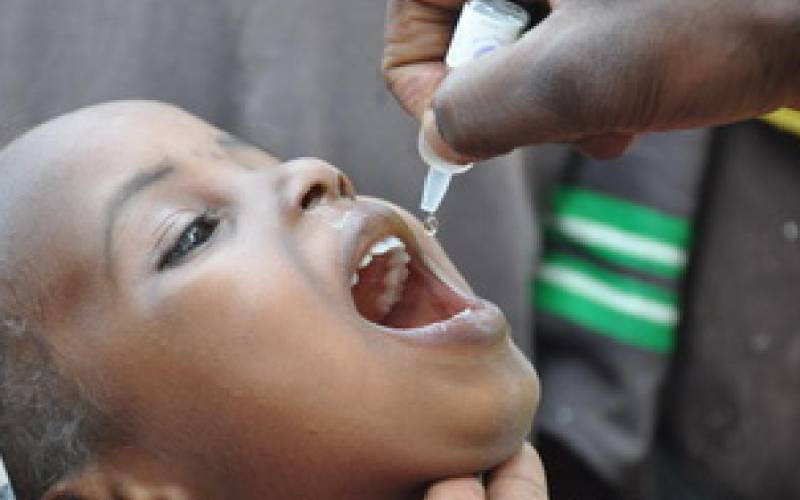
Many parents first rush to the pharmacy when their children fall ill. But pharmacists rarely diagnose the problem before selling drugs. When the children get well, most parents stop the dose until the next illness.
Dr Mirfin Mpundu, Director of ReAct Africa, warns that this practice is leading to antimicrobial resistance (AMR), from which many people are dying of drug-resistant infections, including children.
Speaking during the ReAct Africa Conference in Lusaka, Zambia in July, Dr Mpundu said AMR happens when drugs stop working after bacteria develop ways of medicines "and if one has an infection, and the drugs are not working, the person may die."
Facts First
Unlock bold, fearless reporting, exclusive stories, investigations, and in-depth analysis with The Standard INSiDER subscription.
Already have an account? Login
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.