Most county hospitals cannot afford medicines, food or linen for patients as almost all their money go into paying salaries.
Salaries, low financial allocations to health, unpredictability and delayed disbursements and corruption have been blamed for the crisis in county hospitals.
A report by the Kenya Medial Research Institute (Kemri) and the World Bank-Kenya also blame unpunished corruption in county health departments and failure of the two levels of government to offer sound leadership.
“The overarching finding is that the two levels of government role as a steward in purchasing health care services was weak and characterised by poor accountability,” says the report published last Thursday even as the crisis unfolded.
In a crisis that has been simmering for more than eight months, the Kenya Medical Supplies Agency (Kemsa) in June finally cut supplies to hospitals in Nairobi, Homa Bay, Kisii, Nyamira and elsewhere for unpaid bills.
By the end of June, counties owed Kemsa Sh2.3 billion, with Nairobi having the highest debt at Sh235 million, followed by Narok with Sh104 million.
Health Cabinet Secretary Sicily Kariuki stepped in this week, directing Kemsa to continue supplying drugs as a solution to the problem was being discussed. But the crisis as reported in Kiambu Level Five Hospital, for example, is not just about drugs, with most hospitalsalso unable to purchase non-pharmaceutical supplies.
In Kiambu hospital, inpatients report being told to bring own linen and food while up to four newborns are sharing a bed. Patients say they are being asked to buy drugs from outside the hospital and bring blankets for their admitted relatives.
“We have never seen this kind of thing before,” said a hawker who operates near the hospital.
Kemri, in the report published in the International Journal of Health Planning and Management, had investigated the purchasing arrangements in 10 counties across Kenya.
“For ethical reasons, we have anonymised the counties to protect the confidentiality of study participants,” says the study, which also involved Oxford University.
The researchers tell of shortages of both medical and non-medical supplies in all counties of study.
“Document reviews showed that health products particularly for non-communicable disease, maternal health services, and pediatrics were not readily available,” says the report.
For the shortages, the study first blames what it says is inadequate budgetary allocation to the counties by the national government.
The national Government has been allocating only about four per cent of the national budget to the health sector, way below the ideal 15 per cent.
But even this small budget, the report says, is worsened by delayed and unpredictable disbursements from national to county governments. More delays of funds are also reported between the county governments and the county departments of health.
“Delays and unpredictability in the disbursement of resources from the county treasury to the health department undermined the availability of resources for service delivery,” says the study.
Health wage bill
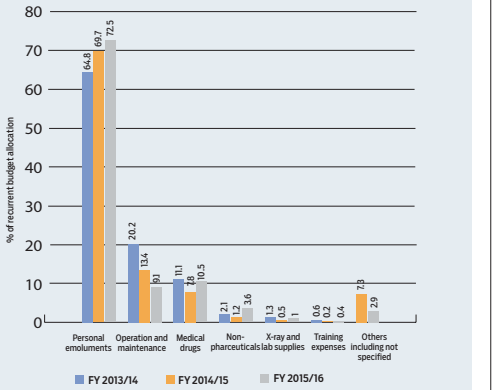
But even when the money is finally received, almost all, more than 70 per cent, goes into the payment of salaries for health workers.
A report compiled under Elkana Onguti, the chief economist at the ministry, said last year that 37 counties had allocated more than the recommended 72 per cent to recurrent expenditure, with almost all the money going into salaries.
Onguti had recommended that counties bring down the health wage bill to between 50 and 60 per cent of their health budgetary allocations. “The current trend is not sustainable,” it said.
This may partially explain why the two governments have been reluctant to employ new doctors even as staff shortages are also being blamed for poor health services.
In the 10 counties, almost all had serious shortages of health workers, with a gap of up to 90 per cent for doctors and more than 60 per cent for nurses.
“We want the County Government to address the shortage of workers immediately,” health workers from Samburu County demanded at a meeting held in Nakuru last week.
To ease the problem of high wage bill and poor health services, the Kemri study is suggesting drastic measures such as ceasing employment of health workers on fixed salaries.
“Such a system may include moving from fixed salaries for all health care workers to hybrid systems that include fee for service by specialists.”
Put against a score of 23 crucial parameters for offering adequate health care to the public, all the counties failed on most of the targets.
This, Kemri says, included poor accountability systems, which allowed corruption to flourish and go unpunished while quality of services was largely unsupervised.
While the county governments require their health departments to institute quarterly audits, this was not being done while those responsible for the failure were never called into account.
“Poor auditing was thought to have contributed towards the increasing reports of corruption in the health department,” says the study.
www.rocketscience.co.ke
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.