More than 1,000 primary school pupils in Busia County learn and play on a disused graveyard. New constructions at Alupe Primary School feature gory scenes of exhumed skeletal bones. Pupils have to be kept away from such scenes to save them from trauma.
Less than a kilometre away from the bustle of the school is what has remained of Alupe, the one time East and Central Africa’s only leprosy and skin disease research centre or leprosarium now converted into a sub district hospital.
At its peak, the centre established by the Colonial Government in 1952 to quarantine patients suffering from leprosy had about 300 patients drawn from all over the region.
Many of them lived at a designated asylum camp nearby. It had farms, churches other social amenities and 10-acre cemetery.
Handouts
Then the school came in 1974 to accommodate a growing population of children from the camp and the exclusive cemetery for leprosy patients was closed down. Busia County Council took over the responsibility of burying unclaimed bodies.
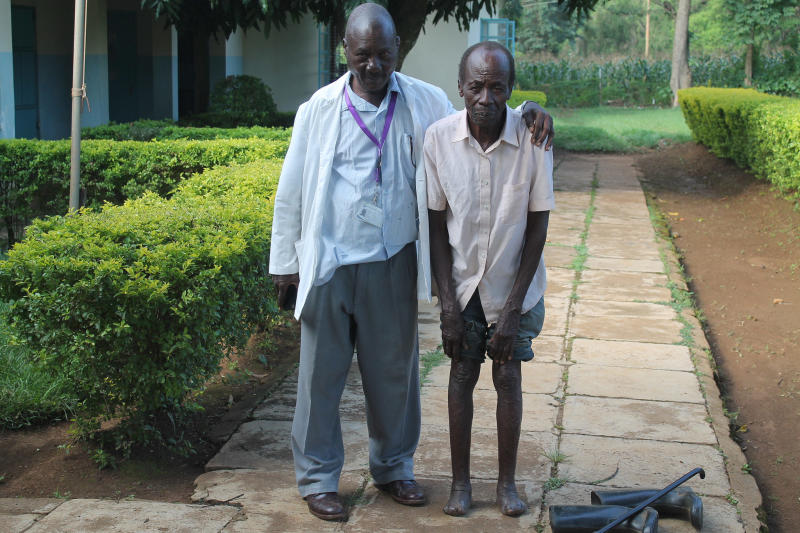
Samson Kiptalam, 68, and Seferio Juma, 73, are the remaining living faces of the Alupe Leprosarium after the camp was demolished in 2002 when donor funding by the Government of Netherlands evaporated with little injection from the Kenya Government.
Francis Amakoye, a Senior Occupational therapist who has worked at the facility since the leprosarium days says the camp’s demolition started in 2002 after supplies that used to come from the Netherlands to cater for confined patients ceased, leaving only drugs for diagnosed cases.
“We used to get everything from food, shoes, ointments, gloves, sandals -- virtually everything the patients needed for free. There were even dairy cattle to supply the patients with milk. All that dried up.
“Many of the over 200 confined patients had left the camp by the time demolition of seven of the eight brick blocks started in 2002. The one block where Kiptalam and Juma live was left to serve as a social relic.”
Kiptalam and Juma are healed but have no home to go to after they were rejected by relatives.
Their survival revolves around the hospital and handouts because they can’t do any meaningful work.
Before they contracted the disease in 1972, Kiptalam was a truck driver on the Mombasa-Bujumbura route.
“It all started with numbness in my feet. I could not feel anything even if pricked by something sharp. The numbness moved to my hands and my health took a truly worrying turn when painless wounds started appearing on my toes and fingers, prompting my employer to suggest that I take time off to seek treatment.
Multiplication rate
“Back home in Nandi, my wife took off with our two young daughters, scared to see my toes and fingers drop. I had developed painless swellings on my face that made me look bad. People avoided me. I was alone and miserable when I went to see a doctor in Eldoret. He told me I could seek treatment only in Alupe and instead of charging me for his services, gave me Sh150 to travel there,” he says.
Kiptalam recalls that he was treated and returned home to Nandi but nobody was willing to give him a job as he did not have toes and fingers.
“I led a dog’s life for 10 years until a septic wound forced me back to Alupe after a sharp object pricked my leg. I have been here ever since. Neither my grown up children nor their mother bother about me,” says Kiptalam who today is on post exposure medication.
Mr Juma, a father of six children who took off with their mother as his condition deteriorated worked as a porter at the Kenya Ports Authority before he was referred to Alupe in early 1980s.
“Doctors truncated eight toes from both my legs that had become numb, an operation they said was meant to contain the bacteria from spreading,” he says.
In a pitiable voice, he adds: “I cannot go home any more. Nobody wants to see me there. My land has been sold by my relatives.
“As for my children, some are working but they have abandoned me, yet it was never my wish to get sick.”
Mr Amakoye says the bacterium that causes leprosy (mycho bacterium leprae) is a cousin to the one that causes tuberculosis -- TB (mycho bacterium tuberculae) albeit with a slower multiplication rate of between 14 to 20 days.
He describes as unfortunate the waning interest in leprosy as attention shifts to TB.
“TB services were benefiting from leprosy services, but things changed with HIV in the late 1980s of which TB became a killer opportunistic infection, relegating leprosy to the back-burner despite the latter’s devastating nature,” he laments.
Amakoye says the reemergence of multi bacillary leprosy cases in children aged between 10 to 15 is worrying at a time TB has stolen the bulk of medical attention.
He notes that Busia County leads with 13 cases out of the known 95 cases nationally.
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.