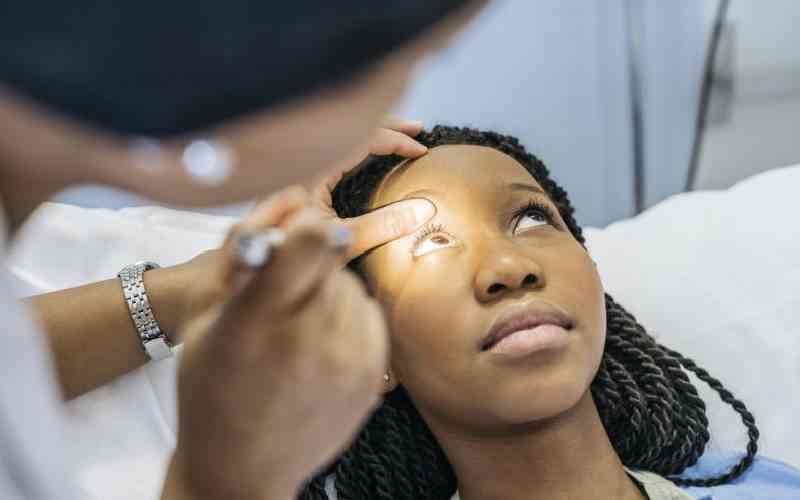
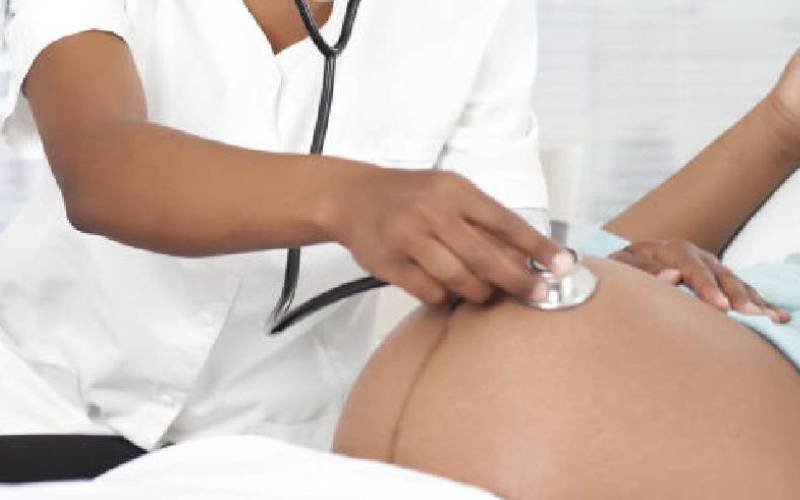
Of the estimated 1.2 million annual deliveries in Kenya, 36,000 have birth defects with about 21,600 dying soon after birth.
Up to 36,000 unborn babies in Kenya have serious defects. And if the pregnancy is not terminated, most of them die soon after birth.
These findings of a new study published last week would roughly mean of the estimated 1.2 million annual deliveries in Kenya, three per cent or 36,000 have birth defects with about 21,600 dying soon after birth.
The study at the Kenyatta National Hospital, the biggest referral facility in the country, followed 500 women through their pregnancies and shortly after delivery.
The pregnancies were closely monitored through ultrasound screening from week 10. Three per cent of the foetuses, the report says were diagnosed with various defects.
Of these, 60 per cent were diagnosed with major abnormalities and the newborns died soon after birth.
The study authored by Callen Onyambu of the University of Nairobi and Norah Taramba of the Ministry of Health says congenital defects are a major cause of newborn deaths in Kenya.
The report says 88 per cent of study participants were non-referrals to KNH and therefore a reflection of the general population.
“But it also means these 21,600 women are made to carry an unviable pregnancy for nine months. This is a health risk and extremely traumatising to the mother,” says Saoyo Griffith, the deputy executive director at the human rights NGO, KELIN.
The study, published in the journal BMC Pregnancy and Childbirth on May 23 recommends screening for birth defects be made part of primary health care and available to all pregnant women.
“This will help diagnose congenital defects earlier and aid in planning for early interventions,” say the authors who describe the study as the first on the subject in Kenya.
“This study highlights the need for Kenyan health systems to go beyond the medical dimensions of illness.”
The authors, while not explicit on what should happen where defects are too severe for the child to survive, report that one such pregnancy in the study group was terminated.
“There was a single pregnancy termination, due to multiple anomalies, some of which were by themselves fatal,” says the study.
The aborted foetus, the report says lacked both kidneys, the bladder, had an abnormal spine and incomplete lungs.
It is only logical, says Saoyo that such a woman be fully informed of the pregnancy status and available options by the attending doctor.
Two options, she says may be open to the woman; either she carries the foetus to term with the knowledge it will not survive or terminate the pregnancy, which is allowed in the current constitution.
The constitution allows for abortion in case the physical and psychological health of the mother is at risk. Other supportive legislature allows abortion in case of emergency treatment.
“This is why at KELIN we want the withdrawn guidelines on safe abortion to be reinstated urgently,” says Saoyo.
The Federation of Women Lawyers (FIDA-Kenya) and Centre for Reproductive Rights have sued the Ministry of Health for withdrawing the guidelines in a case being presided over by a five-judge bench at the High Court.
Already a key expert witness for the plaintiffs, Prof Joseph Kamau of the University of Nairobi has testified that in matters abortion the unborn child has no rights.
Prof Kamau argues that an unborn child is not a person and therefore has no rights.
“It is only after birth that an unborn child becomes a person who the government recognises,” he said.
He says that the life of a mother is more important than that of an unborn baby. The argument is contrasted by the constitution, which recognises life to start at conception.
“That may be so but in this case we are talking about some pregnancies that are not viable and pose a health risk to the mother,” says Saoyo.
The human rights advocate cites the Health Act 2017 currently being operationalised, which in Chapter Six allows safe abortion if the foetus is incompatible with life.
The Act says in part: “Every person has a right to reproductive health care, which includes access to treatment including for abnormal pregnancy conditions.”
The contested document published in 2012 guides health workers on among others how to manage risky, abnormal and unwanted pregnancies.
The lobby groups insist that it is important that the ministry gives direction on when health workers should provide safe and legal abortion.
Lola Wambua, 71 of Tassia Catholic Church in Embakasi, Nairobi says man or woman, none has the right to decide which child live or dies.
“Not even a paining mother, has the right to bend the divine will of God: the Church must resist this arrogance,” she told the Saturday Standard.
But while the KNH study may be news to Lola and other poor families; upmarket women are paying as much as Sh100,000 for the testing of foetuses for genetic disorders outside Kenya.
The women are sending blood samples to laboratories in the UK, US, South Africa and India to investigate whether the babies they carry have genetic disorders such as the Down syndrome, Patau syndrome or Edwards syndrome.
On knowing they may prepare psychologically to live with the problem, or abort the foetus all within Kenya laws.
www.rocketscience.co.ke
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.