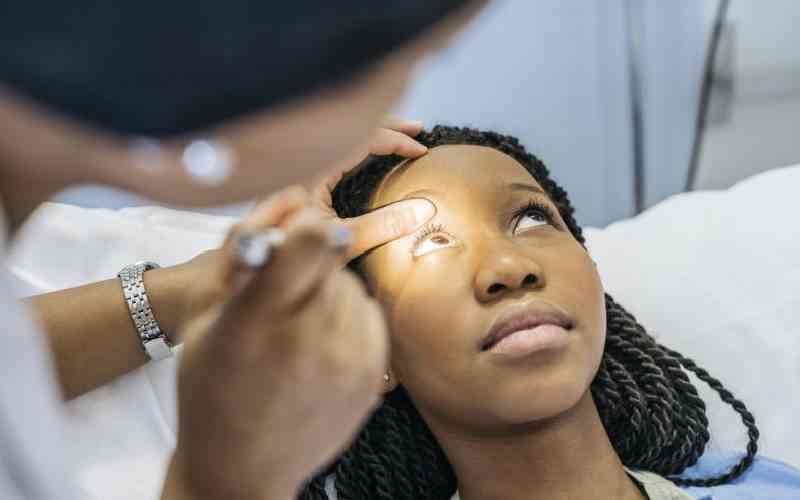
When HIV first became known to the world in the early 80s, the fear of the disease caused negative feelings towards those who tested positive for the virus.
While some people believed that only certain groups of people could get HIV, others made moral judgments about those who took steps to prevent HIV transmission. Many others believed that people deserved to get HIV because of their choices.
Now, 38 years after the first HIV case was reported, we know these negative feelings as stigma.
Despite efforts to educate the public about the virus, Kenyans are still grappling with stigma. This time, it is happening in healthcare facilities, sometimes under the watch of the professionals who are trained and trusted to prevent it.
There has been evidence on HIV prevention and treatment but some persons living with HIV decry that stigma and discrimination persist and they believe this could be one of the causes of the lack of adherence to treatment by some of them.
In an interview with The Standard, Doreen Moraa, a HIV/AIDs advocate said that some health facilities, places that have been known or perceived by many as a safe space, have not lived up to their name if the reports are anything to go by.
"A lot of times most people have expressed frustrations that the healthcare workers treat them badly, or talk in an unfriendly manner. Healthcare set-ups are supposed to be places where one can go when life is overwhelming, or when stigma is happening. Sometimes when you miss a dose or you do not go to clinics, they call you out without even attempting to find out what the problem was," Ms Moraa said.
She said if one found stigma in one health facility, he or she might not gather enough courage to walk into another facility for fear of more stigma and that could be one reason why some may lose adherence.
- HIV funding falls short of targets as millions of lives hang in the balance
- State to receive 110,000 doses of injectable HIV prevention drug
- Resounding success: How new surgery at KNH is restoring children's hearing
- Pharmacy-based PrEP emerges as key in Kenya's HIV fight
Keep Reading
Further, she expressed the fact that although some healthcare providers are overwhelmed, there was a need to exercise caution when handling people living with HIV especially by regarding their levels of acceptance of their status.
"I might have been on ARVs for the last 17 years and the doctors expect that I should be adaptive because one of the causes of stigma is when one has not achieved viral suppression yet you have been on treatment for a while."
She explained that a doctor might give a patient such pressure without finding out why they have not achieved viral suppression or why they have had opportunistic infections. Some doctors, she said, resort to changing the line of treatment, instead of addressing the issues leading to viral spike or lack of viral suppression.
According to Moraa, there is need to create a friendly environment for young people and mothers who are a key population in reducing HIV infection.
"For example, if you are a mother living with HIV and your viral load has spiked, and when you go to the hospital, they call other nurses, oh come and see this one, she is not taking her treatment, she wants to spread the virus to her child, without even asking why she has not been to the hospital. What if she did not have fare to go to the hospital?"
According to Burgwen Muthoka, the coordinator of the Rescue Team for HIV/AIDS in Kibwezi Makueni County, some of the healthcare providers lack the proper communication skills required when handling people living with HIV.
He said that some of his team members have complained that they have to brace themselves to face some healthcare providers, something that has made many stay away from the hospitals.
"Instead of calling out the healthcare providers, we have instead been doing frequent sensitisation workshops where we encourage them to be friendly with the people living with HIV, help them understand why they need to adhere to their medication and be more understanding as most of them have not yet fully accepted their situation, so we don't want them to feel like they are being judged for getting infected."
Kenya PLWHIV stigma index report 2021 indicates that the respondents reported various forms of stigma for HIV-related care at the health facilities including gossip or talking badly, disclosure of respondents' HIV status without their consent, denial of dental care, physical abuse and advice not to have sex and verbal abuse.
Stigma related to gossip and talking badly was at 14 per cent for men and 13 per cent for women, disclosure without consent at 12 per cent for both men and women and avoidance with men at 10 per cent and women at 9 per cent, physical abuse and advice not to have sex at 11- 14 per cent and verbal abuse for both men and women at 10 per cent.
According to the National Syndemic Diseases Control Council (NSDCC) formerly the National AIDS Control Council, the above data indicates that stigma and discrimination are still being experienced at the health facility level.
NSDCC states that there has been training and sensitisation of healthcare workers on the rights of people living with HIV and the need to deliver services devoid of judgmental attitudes and prejudices.
"Healthcare workers are sensitised that they should not enforce compliance -- that is telling the persons living with HIV what to do and for them to do it without question but rather work hand in hand with them to achieve treatment success, taking into consideration their situation such as work, level of acceptance, self-stigma, disclosure, beliefs, family and community situation."
Additionally, NSDCC states that people living with HIV have been sensitised on their human rights to recognise when their rights have been violated and take the necessary steps to ensure they get redress including lodging complaints within the management of the health facilities.
The Ministry of Health has also devised the Differentiated Service Delivery model where some members of one community form a group, and can collect drugs for the other members in a bid to reduce the number of hospital visits for all the members, time spent at the facility and the transport costs.
Members who qualify to be part of this model are those that have achieved viral suppression, have been on treatment for more than one year, are not pregnant, do not have advanced HIV disease, are not a child or adolescent and have not missed clinical appointments.
The rest of the team members will only visit the hospital facility when they are due for blood work such as viral load tests or if they feel unwell.
Additionally, the National Empowerment Network of People Living with HIV (NEPHAK) that has been conducting surveys states that the national stigma index 2021 was at 22.3 per cent where they have been giving health talks by people living with HIV, and ensuring that they are also part of staffing for health facilities such as mentor mothers.
"We also monitor, document and refer cases of human rights violations and stigma in health facilities and share with the relevant authorities," says Nelson Otwomwa, the Executive director at NEPHAK.
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.