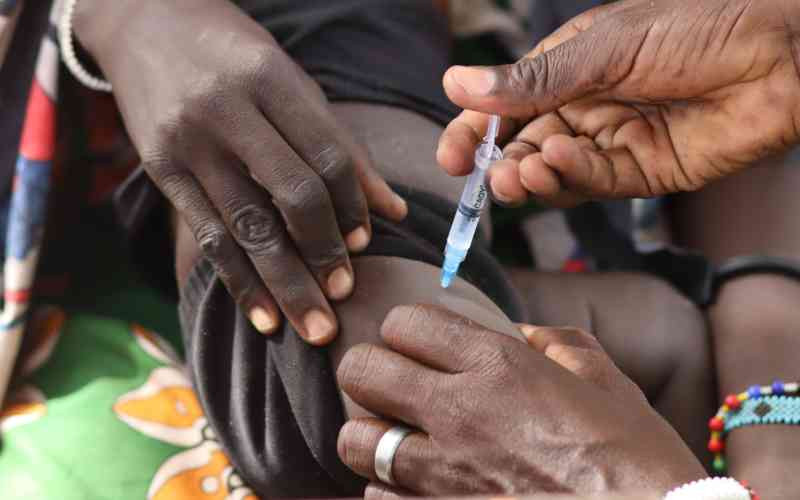
Kenyans in the US have been listed among immigrants from five countries at highest risk of developing and spreading tuberculosis.
This means those already in the US or planning to move there from Somalia, Ethiopia, Myanmar, Liberia and Kenya, in that order, will face more scrutiny and surveillance.
Facts First
This story continues on The Standard INSiDER. Subscribe now for unfiltered journalism that holds power to account.
Already have an account? Login
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.