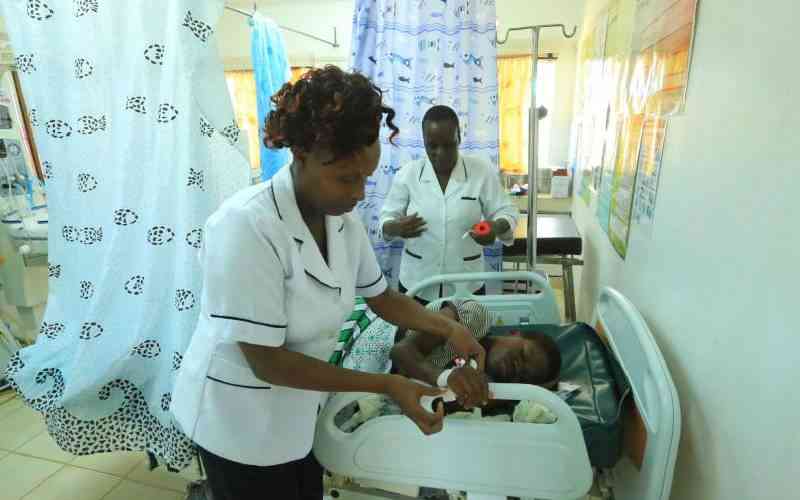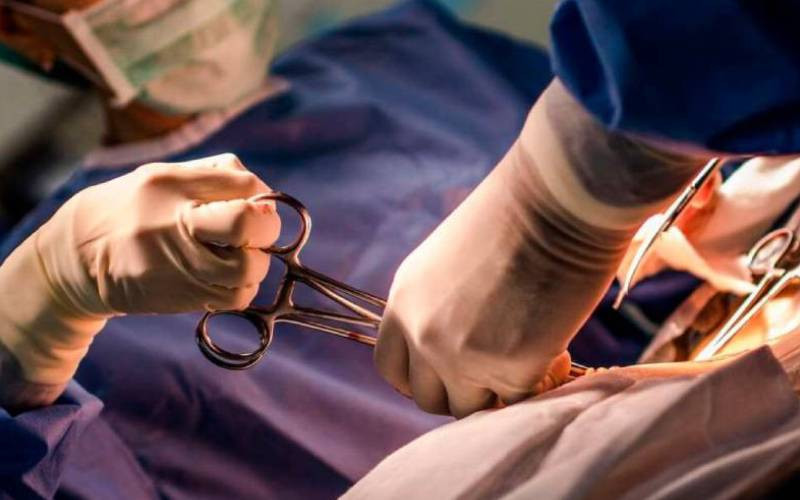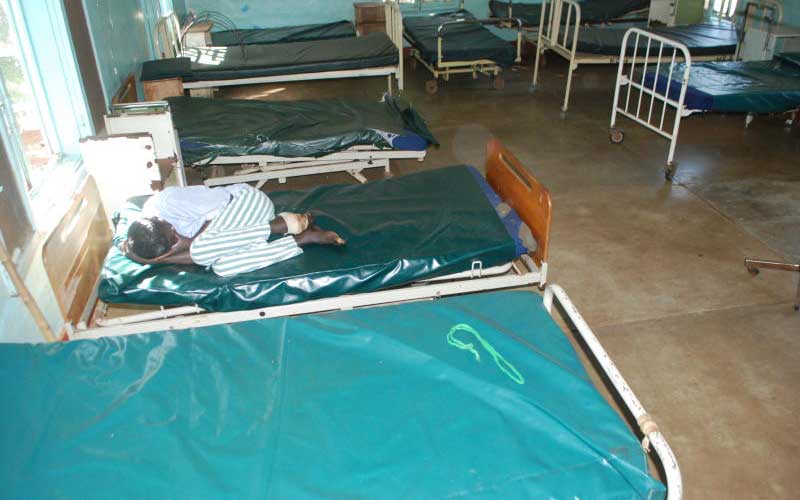
The withdrawal of health care services during the now frequent health workers strikes has no effect on patient deaths.
Medical experts assessed 6,396 deaths during a seven-year period involving six strike cycles and now report no impact on hospital fatalities whether health workers strike or not. One reason for this, the experts suggest may be because the quality of care being offered in public hospitals is too poor to make any difference.
“One explanation for recording no change in mortality between strike and non-strike periods could be related to sub-optimum quality of services being provided during regular operation of health facilities,” the study says.
The study involving world-class academic institutions including Yale University, US, London School of Hygiene & Tropical Medicine, UK, Imperial College London, UK and University of Oxford, UK was led by KEMRI-Wellcome Trust Research Programme Kilifi.
The researchers had investigated the impact of doctors and nurses’ strikes on all deaths between 2010 and 2016 in Kilifi County.
While they do not generalise, their report published last week (May 22, 2019) in The Lancet is a major indictment on the kind of health care millions of Kenyans get in public hospitals.
Other recent studies have assessed the number of inpatients who missed care due to strikes and hypothesised that many could have died at home. “If health-care provision is compromised under normal circumstances, the effect of its cessation would be marginal,” says the study.
Strikes, they explain have also been associated with a reduction in exposure to potentially harmful interventions, such as elective surgical procedures and hospital acquired infections especially with infants.
Threats to sue
For similar reasons, last week the Kenya National Union of Nurses threatened to sue the Kirinyaga county government over hospital acquired infections.
Union, Secretary General, Seth Panyako alleged five nurses got infected with hepatitis while seven others caught cholera at Kerugoya County Referral Hospital. “The hospital is very dirty… and our doctors cannot work in such an environment; already some have acquired incurable diseases,” said Dr Gor Goody, of the Kenya Medical Practitioners, Pharmacists and Dentists Union while launching another strike in Kirinyaga on Wednesday.
On the same day the Kilifi study was published, it got strong support from Dr Muma Nyagetuba, and Dr Mary Adam both of AIC Kijabe Hospital. “Your results could point to issues surrounding quality of care available to Kenyans at government facilities,” the duo wrote in the same journal.
The duo cited lack of drugs, minimum necessary equipment, and insufficient ratios of doctors and nurses to patients as the main issues bedeviling public facilities.
The two were especially disturbed that the death rates among newborns were similar whether a health care worker was present or not. More evidence published in March 2019 by Moi University, Eldoret, Indiana University, US, and the Academic Model Providing Access to Healthcare suggested many home births in Kenya may be safer for newborns than hospital deliveries. The researchers had analysed 36,375 deliveries in Kenya for a four-year period, and reported that infants delivered in hospital had higher risk of dying than those delivered at home due to poor quality care in hospitals.
Perinatal mortality
The study published in March in the journal Seminars in Perinatology concluded: “Infants born in facilities had a 41 per cent greater risk of perinatal mortality than infants born at home.”
Coincidentally, on Thursday the KEMRI-Wellcome Trust tweeted a policy brief on newborn care in Nairobi.
The brief says of 31 hospitals that provide 24/7 inpatient neonatal care in Nairobi, only seven had at least 80 per cent of the requisite capacity to give patients adequate care.
Of the 24,000 seriously ill newborns in Nairobi annually only 24 per cent or 5,760 are likely to access a hospital that provides adequate quality care.
It gets even scarier with a study published last year showing stroke outpatients were likely to survive longer than inpatients treated at both Kenyatta National Hospital and Moi Teaching and Referral Hospital.
Inpatients, the study appearing in the journal Cerebrovascular Diseases had an almost four-fold increase of dying compared to outpatients and this increased with longer stay at the hospitals.
Rattled by recent patients’ adverse events in several hospitals, the Cabinet Secretary for Health Sicily Kariuki has called for a nationwide audit of all health facilities.
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.