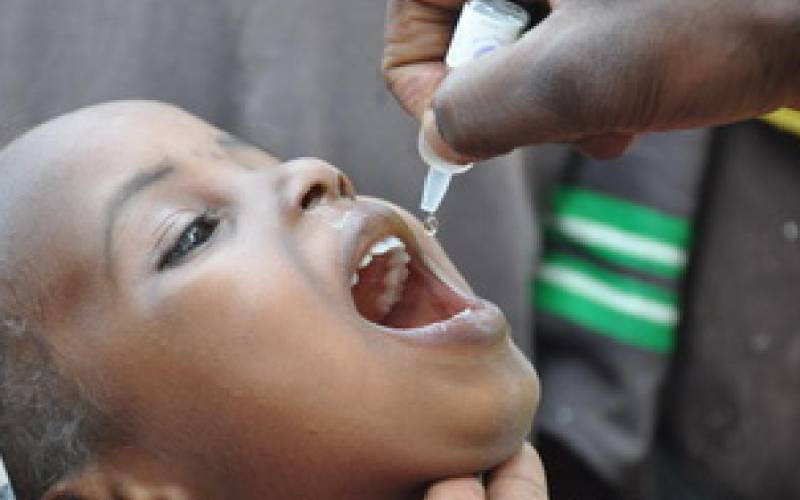
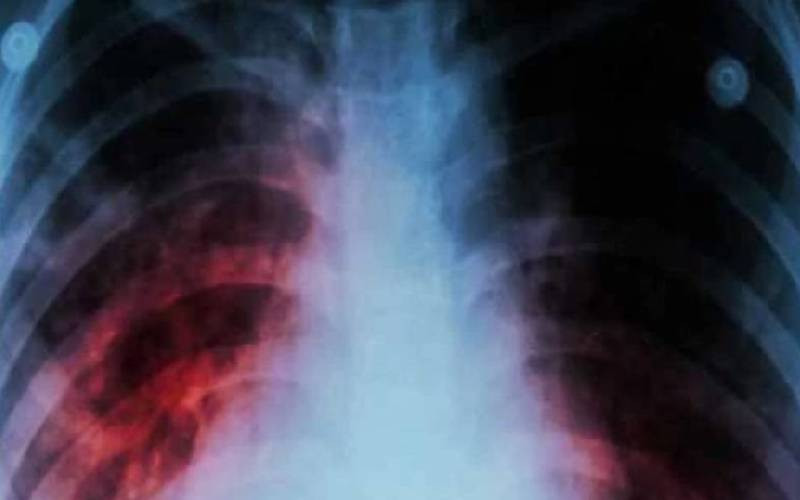
There is a silver lining in the fight against Sexually Transmitted Infections (STIs) for Kenya and the globe, following announcement of new guidelines for testing and diagnosis of four highly transmitted diseases.
The guidance released by WHO include target product profiles (TPPs) for point-of-care diagnostic technologies for diagnosing syphilis, chlamydia, gonorrhoea and trichomonas vaginalis.
Guidance on STIs was announced by WHO, during the ongoing STI and HIV 2023 World Congress, in Chicago. The guidance is aimed at facilitating development of quality STI diagnostics.
TPPs according to WHO help to ensure that products are designed and manufactured to meet the clinical needs of populations at risk and are "fit-for-use". Point-of-care tests can lower health-care costs, reduce waiting times, speed up initiation of and increase the accuracy of treatment, and improve patient follow-up of patients.
Additionally, point of care diagnostic testing for STIs including HIV provides up to date information on how to isolate, detect, and diagnose STIs, including HIV.
The guidelines were issued at a time Kenya and the globe are reporting increased cases of STIs.
Globally, more than one million new STIs are acquired every day, posing a significant global health challenges.
However, monitoring and understanding the trends of new STIs in low- and middle-income countries (LMIC) are hindered by limited access to diagnostic tests.
"Early testing and diagnosis are key in stopping the spread of STIs. When left untreated, certain STIs can lead to long-term irreversible outcomes and some can be potentially fatal," said Dr Teodora Wi, Lead for Sexually transmitted infections of the WHO Global HIV, Hepatitis and STIs Programmes.
"Our new guidance can help make low-cost point of care tests for STIs more accessible, enabling improved data collection and quality delivery of STI services for people in need".
Dr Stephen Kaliti, a consultant Obstetrician Gynaecologist and Director of public health and medical services, state department for public health and professional standards, said the WHO stipulated guidelines are important in treatment and management of patients with STIs.
The TPP technology, he explained,-"Is user centred, has an expanded range of pathogens to detect in a single testing episode, may be more efficient and give results faster for earlier diagnosis and rapid initiation of treatment"
In Kenya, testing of chlamydia and gonorrhoea is done like pap smear where a speculum is put in the private area, and have a high vaginal swab removed for laboratory tests.
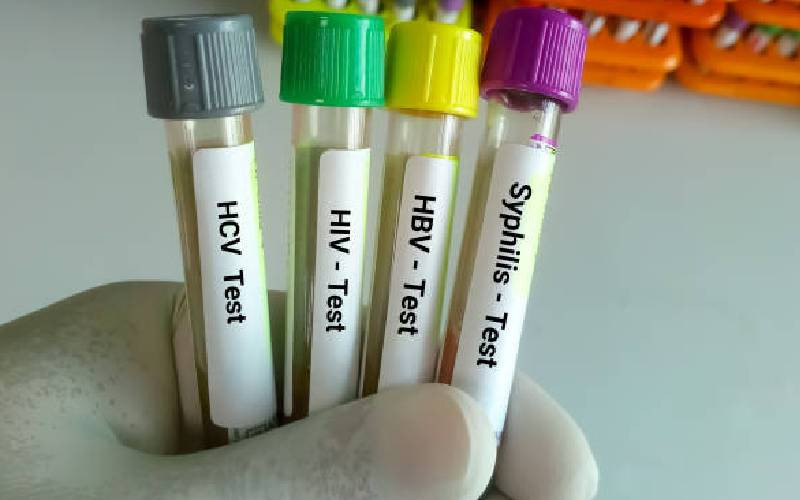
Though Kenya conducts advanced tests and diagnosis to four leading STIs namely syphilis, chlamydia, gonorrhoea and trichomonas vaginalis, the tests are done in high-end laboratories, according to Kaliti.
For syphilis, various methods for tests are used, for example, rapid plasma reagin (RPR), the Venereal Disease Research Laboratory (VDRL) test and the toluidine red unheated serum test.
The newer methods use genetic probes, (PCR), are more exact, rapid and specific to the genetic makeup of the pathogen but may cost more.
The preferred current test for chlamydia is Nucleic Acid Amplification Test (NAAT), previously ams routinely microscopy are used to see" clue cells" or blood tests for the antigens against chlamydia.
"We are ready to embrace the technology of testing STIs, according to WHO guidelines, but may be more costly," said Kaliti. "There are other tests in Kenya, but at high-end labs. The challenge is to lower the cost and make them routine or deploy them for public health system use".
On his part, Dr George Moses Ogweno, a fertility and IVF specialist, said TPPs for point of care diagnostic technologies will improve diagnosis, treatment and reduce spread of infections.The new testing technologies, he said, will also prompt quality management of infections.According to Dr Ogweno STIs are one of the major causes of infertility, currently being witnessed among individuals in reproductive age."If patients are diagnosed and treated on time, especially at the point of tests, we shall not have referrals and long wait to have patients treated," said the fertility expert.Ongweno said the new diagnostic as per WHO guidelines should be done at lower hospitals like dispensaries, and target disadvantaged groups like slum areas where STIs could be a major challenge to diagnose."TPPs for point care diagnostic technologies is something that is encouraging because most of the time, we have a challenge on turn around time," said Dr Ogweno.
He said the guidelines will also reduce stigma, as patients privacy will not be infringed because results will be instant, unlike the current challenge where access to rapid tests used to test chlamydia and gonorrhoea are used."With better testing modalities, it will be easier, we see taking vaginal swabs as very intrusive, and especially with adolescents who are mostly uncomfortable. Some cultures also make patients reluctant to undergo tests," added Dr Ogweno.
"It is a worrying trend that individuals who undergo tests do not pick results, because of unknown fears, an issue that will be handled by new testing modalities,"The expert emphasised that technology will also help address some major causes of infertility at a much earlier stage.
Dr Kaliti added that Kenya is experiencing a rise of STI's, emergence of resistant strains and a relaxation of use of barrier protection during intercourse.
"There is an increase in casual and unprotected sexual encounters, a rise in infertility attributable to STI's," said the official.
To reduce STIs infections, the Ministry of Health encourages abstinence, public awareness, protected intercourse, deliberate surveillance for STIs and up tick of population screening for STIs, treatment guided by sensitivity of medicine used to treat the specific infection, regulation of over the counter self treatment for STIs.
"There should be responsible engagement in intimate actions and adherence to a single uninfected intimacy partner," added Kaliti.
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.