Africa, like other continents, has a problem with Anti-Microbial Resistance (AMR). But Africa stands out as it has not invested in capacity and resources to determine the scope of the problem, orhow to fix it.
For starters, consider Staphylococcus aureus, which is the source of a skin infection that can turn deadly if resisted by drugs.
Estimates on the most common resistant variation, methicillin-resistant Staphylococcus aureus (MRSA), exceeds 100,000 deaths globally in 2019.
But up until recently, we did not have a solid grasp on how much of a problem MRSA - or any other antimicrobial resistant pathogen - was in Africa.
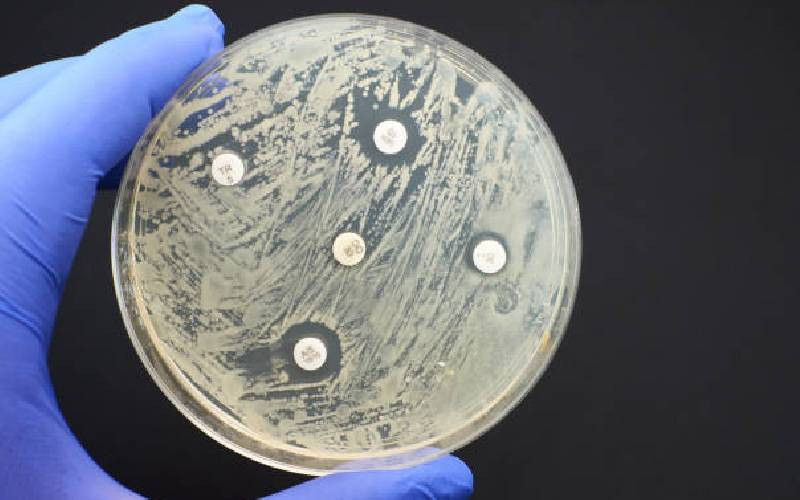
It turns out, after testing 187,000 samples from 14 countries for antibiotic resistance, scientists found that 40 per cent of all Staph infections were MRSA, but we still don't know what's causing the bacteria to become resistant, nor the full extent of the problem.
We are failing to take AMR seriously, perhaps because it is not glamorous and relatable.
The technology that we currently use to identify resistant pathogens is not fancy or futuristic looking. Combating AMR does not involve miracle drugs, expensive treatments, or fancy diagnostic tests. Instead, we have bacteria and other pathogens that are commonplace and have learnt how to shrug off the good old medicines that used to work.
The global health and pharmaceutical industries do not seem to consider solving this problem as profitable compare with the speed with which vaccines for Covid-19 were found complete with government subsidised diagnostics to end the pandemic.
- Animal welfare group expands efforts to control rabies with new Watamu branch
- New study maps high drug resistance in Kenya and other 13 African countries
- Revealed: Cerelac baby food contains high sugar levels
- She kept working: Farmer's long and painful fight with brucellosis
Keep Reading
Why can't the same be done for AMR, yet the World Health Organisation (WHO) has repeatedly stated that AMR is a global health priority - one of the leading public health threats of the 21st century?
A recent study estimated that in 2019, nearly 1.3 million people died because of anti-microbial resistant bacterial infections, with Africa bearing the greatest burden of deaths. A high prevalence of AMR has also been identified in foodborne pathogens isolated from animals and animal products in Africa.
Collectively, these numbers suggest that the burden of AMR might be on the level of - or greater than - that of HIV or Covid-19. The growing threat of AMR is likely to take a heavy toll on Africa's health systems, but the paucity of accurate AMR information limits our ability to understand how well commonly used anti-microbials actually work.
This also means we cannot determine the drivers of AMR infections and design effective interventions in response.
Data from our recent project on many of the scariest pathogens in 14 countries, gave insights into the under-detected and under-reported depth of the AMR crisis in Africa. Less than two per cent of the medical labs in the 14 countries examined can conduct bacteriology testing, even with conventional methods that were developed more than 30 years ago.
While a strengthened workforce is critical, many health facilities in Africa are coping with interrupted access to electricity, poor connectivity, and serious, ongoing workforce shortages.
Containing AMR means we have to fix African health systems. The work starts now.
-Dr Pascale Ondoa is the Director of Science and New Initiatives, African Society for Laboratory Medicine and Dr Yewande Alimi is the Africa Centre for Disease Control AMR programme coordinator.
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.