Having a sexually transmitted infection is a bad enough experience on its own. Usually though, it is nothing that a treatment course from your doctor won’t help clear off. And then you promise yourself to be more careful in the future. But then, the disease-causing microorganisms are evolving, too, and thanks to this, turn into what scientists call untreatable gonorrhoea. Super gonorrhoea, others call it. And it is on the rise, right here in Africa.
But hold on, before we explore this super bug, let’s examine a few facts. Gonorrhoea is the most common sexually transmitted disease.
The World Health Organisation approximates that 11.4 million gonorrhoea cases occur annually in the African region, and warns of the emerging threat of ‘untreatable’ gonorrhoea. Those of us in the public health sector understand quite clearly that gonorrhoea is quite a stubborn disease.
How the super bug developed
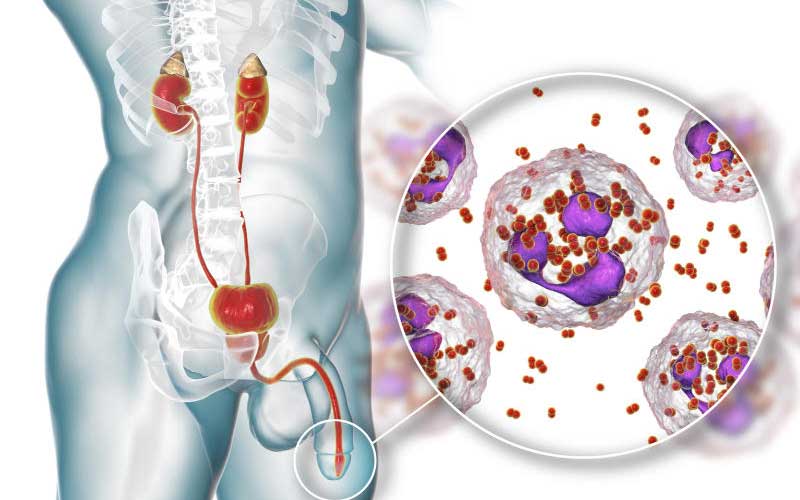
Caused by a bacterium known as Neisseria gonorrhoea, the disease has notoriously developed resistance to outsmart the class of antibiotics used to treat it. The new resistant strains are reported to be as a result of inter-species recombination of genes between the main causative bacterial agent, N gonorrhoea, and other commensal strains of the same genus. This alarming recombination continues to stress already-dwindling treatment options, and the WHO is concerned about a near future with a super bug that causes untreatable gonorrhoea. The bug infects the cervix, uterus and oviducts (fallopian tubes) in women, and urethra in both men and women. It can also cause infection in the eyes, mouth, throat and rectum.
How do you get it?
Sexual contact in the main mode of transmission of gonorrhoea. Either through the penis, vagina, mouth or anus, an infected partner can pass it along. For a man, no ejaculation is needed for you to transmit or acquire it. In addition, infection does not guarantee immunity. That means one can be re-infected even after previously successful treatment against gonorrhoea. Infected mothers can also pass it to their babies during childbirth.
Why you should be worried
The absence of a vaccine for preventive purposes makes us rely on antibiotics as the only means of managing gonorrhoea. In Kisumu, between 2000 and 2010, there was a 50 per cent increase in resistance of gonorrhoea to ciprofloxacin, a drug that was previously used to treat it. This is according to research done on antibiotic resistance in gonorrhoea in people living in Kisumu.
Ciprofloxacin belongs to a class of antibiotics known as fluoroquinolones. After reporting fluoroquinolone resistance in western Kenya in 2009, the coast region in 2011 and in Nairobi in 2012, the national treatment guidelines for treatment of gonorrhoea were revised to include a class of antibiotics called cephalosporins. Even though adherence to medication will treat the infection, it will not restore any permanent damage caused by the infection.
Origin of the strain
A study published in the Oxford Academic Journal of Antimicrobial Chemotherapy showed that antimicrobial resistance developed first in the WHO Western Pacific Region (which includes China), followed by international spread. A survey by Kenyan scientists done over a period of four years, from 2012 to 2015 in Nairobi, found that ceftriaxone was still a useful antibiotic in the treatment of gonorrhoea. Other antibiotics that were still shown to be useful include cefixime, spectinomycin and azithromycin.
A majority of both men and women with gonorrhoea are asymptomatic. In men, symptoms include:
A white, yellow or green urethral discharge
Pain when urinating
Scrotal and testicular pain.
In women, symptoms are sometimes mistaken for vaginal or bladder infection. Most women experience:
Increased vaginal discharge
Pain when urinating
Bleeding between periods
In both men and women, rectal infection may manifest through:
Itching
Painful bowel movements
Soreness and bleeding.
Sometimes one develops a sore throat.
Permanent health problems
Pelvic inflammatory disease (PID) in women can occur with infection that spreads out into the uterus or fallopian tubes.
PID subsequently causes chronic pelvic pain, damaged fallopian tubes, which is enough to increase the risk of ectopic pregnancy and infertility.
In men, untreated gonorrhoea is also associated with infertility.
When gonorrhoea spreads into the blood, it can cause a life-threatening condition known as disseminated gonococcal infection (DGI). This is a condition characterised by arthritis and tenosynovitis. It also increases one’s risk of transmitting or acquiring HIV.
What increases the risk to gonorrhoea infection?
Lack of or incorrect use of barrier protection in sexual exposure with an infected partner
Male homosexuality
Multiple sex partners
Dr Supriya Mehta advises on the use of region-specific guidelines for the management of the disease.
“Many countries have treatment guidelines for gonorrhoea, but they need to be specific to local epidemiology and microbiology.”
When diagnosed with gonorrhoea, furnish your doctor with an adequate sexual history to avoid treatment failure and to foster effective treatment of asymptomatic patients.
A sexually active man who has sex with men or is bisexual should go for gonorrhoea screening every year. So should a sexually active woman, young or old, who has multiple sex partners or a partner who has an STI.
Nancy Nzalambi is a research scientist with NHIF
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.











