×
The Standard e-Paper
Fearless, Trusted News
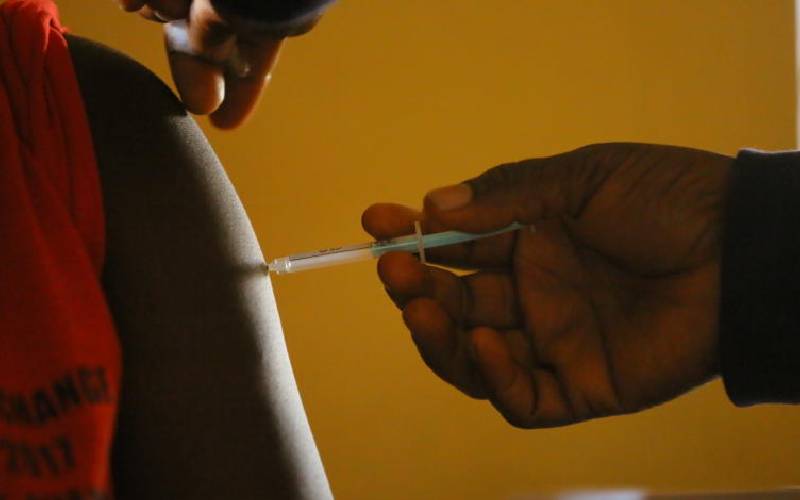
After four decades of tireless research, groundbreaking developments in HIV vaccine research are offering new hope to scientists and the global health community alike. An effective HIV vaccine would prevent new HIV infections and could therefore play a powerful role in bringing the Aids epidemic to an end.
While the HIV vaccine journey seems to have taken long, research done to date has yielded fruits in the development of a Covid-19 vaccine and paved the way for innovations that bring the field closer to an HIV vaccine.