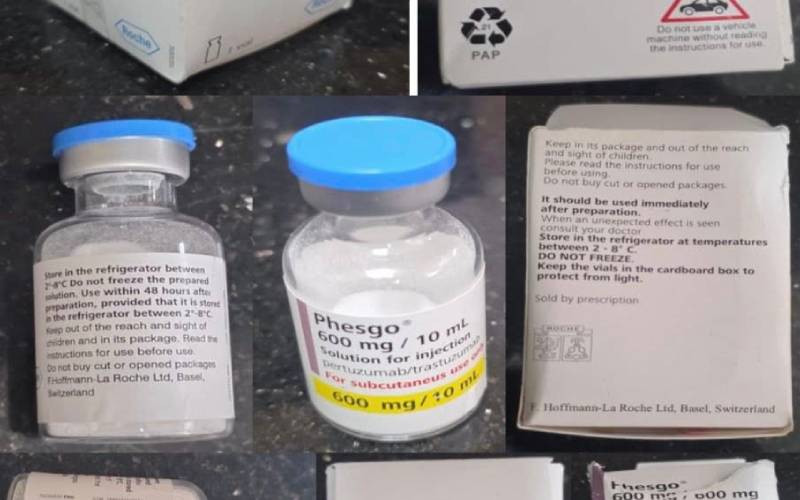
Drugs bought over the counter, like painkillers and antibiotics can result in detrimental health side-effects.
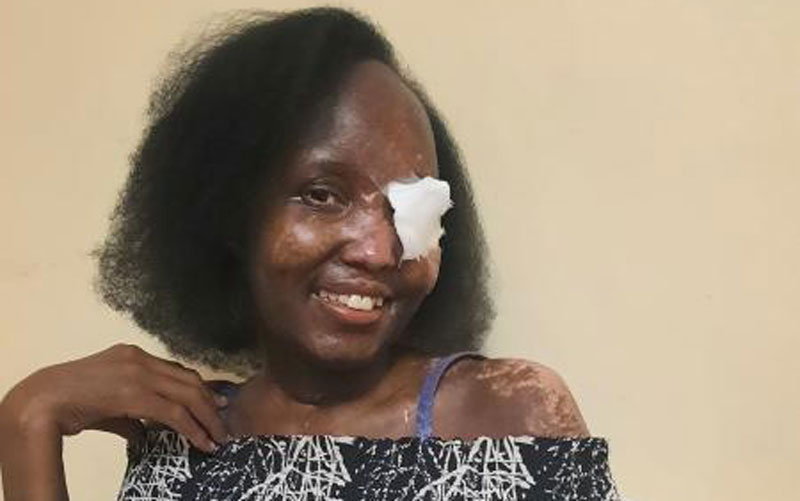
For Christine Hannah Gitaka from Murang’a County, they resulted in Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis (SJS/TEN) after the 39-year-old reacted to her prescription medicine.
It all started when hitting her head left her epileptic in 2009.
Facts First
Unlock bold, fearless reporting, exclusive stories, investigations, and in-depth analysis with The Standard INSiDER subscription.
Already have an account? Login
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.