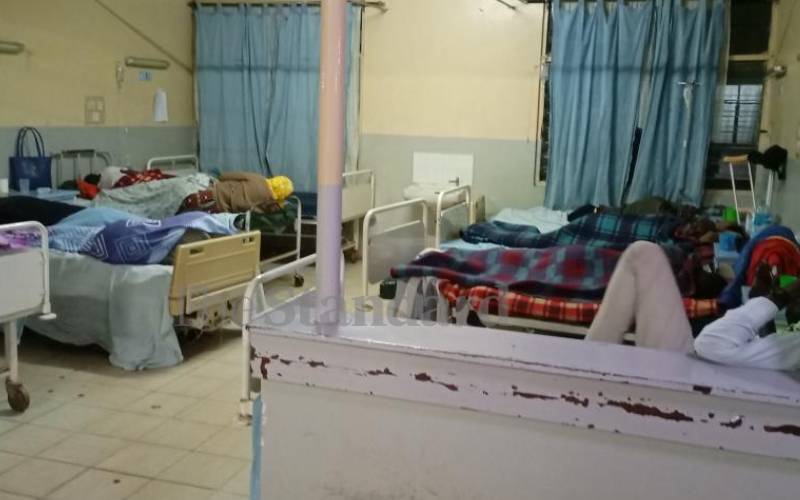
The situation at one of the wards at Kapsabet County Referral Hospital. [Mercy Kahenda, Standard]
It is 4.45pm on a Tuesday at Kapsabet County Referral Hospital and multiple patients flock the casualty area, majority in critical state. But at the consultation room, patients crowd due to delays caused by shortage of basic supplies such as syringes, cotton wool and antibiotics. Patients have to buy them from private chemists.
At 5.12pm, a patient in his early 30s is brought in by an ambulance. He lies unconscious on the stretcher. Anxious looking neighbours accompanying the patient inform The Standard that he attempted suicide.
Facts First
This story continues on The Standard INSiDER. Subscribe now for unfiltered journalism that holds power to account.
Already have an account? Login
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.