×
The Standard e-Paper
Join Thousands of Readers

Audio By Vocalize
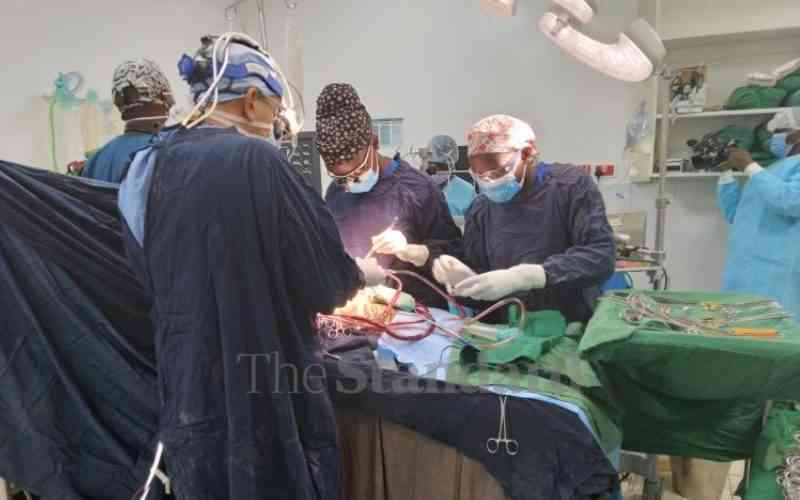
Ten years ago, disturbing media reports revealed that heart surgery patients had been on a surgical waiting list for up to two years before receiving life-saving intervention.
The country's main challenge at the time was a combination of a shortage of heart surgeons (cardiothoracic surgeons) and theatre facilities. Although some progress has been made in both areas since then, the situation remains desperate.
