×
The Standard e-Paper
Stay Informed, Even Offline
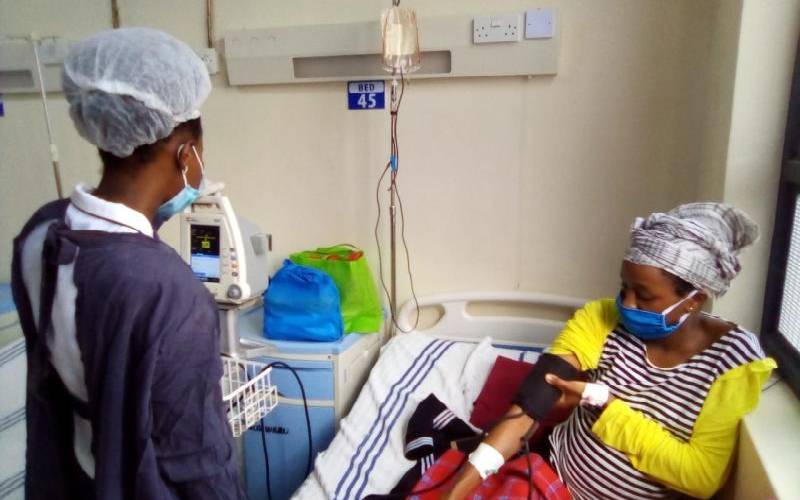
On June 9, 2020, Betty Kiplagat, a first time mother at 26, had a safe delivery and was elated as she held her bundle of joy.
Sadly, as she cuddled her baby at Chemolingot Hospital in Baringo, the mother begun bleeding excessively and became unconscious.