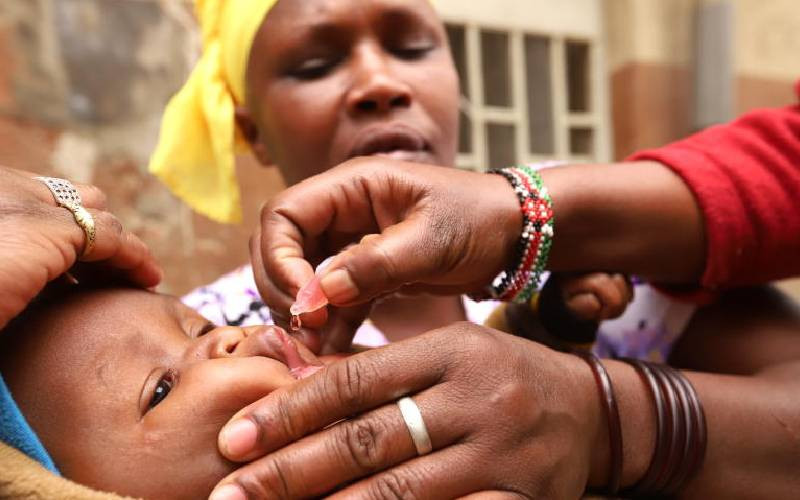
The incoming government will be staring at a health financing crisis as major donors gradually pull funding for malaria, HIV and Aids, reproductive health, blood services, immunisation, TB and drugs in the next five years.
For instance, immunisation programmes funded by Gavi, the vaccine alliance, will end in 2027. And the effects are already being felt with reported shortage of contraceptives, condoms, ARVs and testing kits.
Beatrice Kiprop, a mother of three from Eldai village in Nandi, for instance, has unsuccessfully tried getting contraceptives from government facilities. "I have been buying family planning pills at a private chemist for two months now. I spend about Sh1,000 every month," said Ms Kiprop, a peasant farmer.
Dr Daniel Mwai, a health economist, says donors are pulling out because Kenya has graduated from being a low-income to a middle-income country, which is above the category of countries in need of funding.
Family planning services is among interrupted donor programmes in the face of increased demand. Data from the Ministry of Health indicates that about 6.1 million women are using modern methods of contraception, an increase from four million in 2012.
Dr Ruth Masha, CEO of the National Aids Control Council (NACC), said that family planning services have been affected due to reduced funding by donors, including Global Fund and UNFPA, which gives Kenya 180 million condoms worth Sh25.4 billion annually.
Condoms are also used to prevent the spread of sexually transmitted diseases like HIV and Aids, gonorrhea and Chlamydia.
"Family planning is an area of concern," said Dr Masha. "For a long time, we budgeted, but never allocated. The donor left."
- HIV gains at risk as donors cut lifeline support
- Why 'disco matanga' is to blame for high HIV prevalence
- Health Ministry launches registration for Nairobi Half Marathon ahead of World AIDS day
- Fighting in silence: The untold stories of learners and teachers living with HIV
Keep Reading
As a mitigation, the ministry has been supplying free condoms to groups at risk like sex workers and homosexuals.
Masha, who also chairs the donors' Transition Committee for a self-sustaining healthcare system, said that most donors are currently opting to provide technical support while pushing countries to buy own commodities.
"Donors want countries to use local resources to take care of the gap. But the gap has kept on growing and most of the resources have challenges for big diseases," said Masha.
The USA, which supports HIV programmes through the President's Emergency Plan for Aids Relief's (Pepfar), ended the support in 2019.
Its funding for HIV commodities has been shrinking over the years: from Sh17 billion to Sh11 billion, Sh9 billion to the current Sh7.3 billion. This has affected blood services, leading to inconsistent supply of ARVs and testing kits, which affects the 1.5 million people living with HIV in Kenya, according to 2018 data from NACC.
At least 53,236 women living with HIV receive ARV prophylaxis to prevent transmission to their newborn children.
Dr Mwai said that donors have been reducing their funding to some strategic programme areas which Kenyan needs to focus on.
For instance, to enhance blood transfusion services, the Treasury increased budgetary allocation from Sh200 million to Sh700 million, besides Sh1 billion World Bank grant.
Masha reckons Kenya is slowly transitioning from donor-funding to self-sufficiency in healthcare, more so in HIV, by promoting local manufacturing of ARVs to ease the cost of importation.
With dwindling finances, she says, one has to trade between buying drugs or commodities considering that "if we do not give university students condoms, it will be expensive treating them for HIV, STIs or infertility".
The country is also revamping its supply chain by strengthening the Kenya Medical Supply Authority.
Dr Mwai, however, slammed county governments which receive 70 per cent of healthcare functions, but have prioritiseed the construction of structures.
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.











