What are the chances that you would get a condition that affects only one in 5,000 women globally?
The day Julian Peter discovered she was different from other girls, she had gone to hospital to get her feet checked. They had developed an arch and they hurt so much that she decided to see a doctor.
“The doctor asked me when I last had my period. I was 17, and I hadn’t had any yet.”
That answer seemed to jolt the doctor who put her through a series of tests and a surgery that would lead to a discovery that has changed her life.
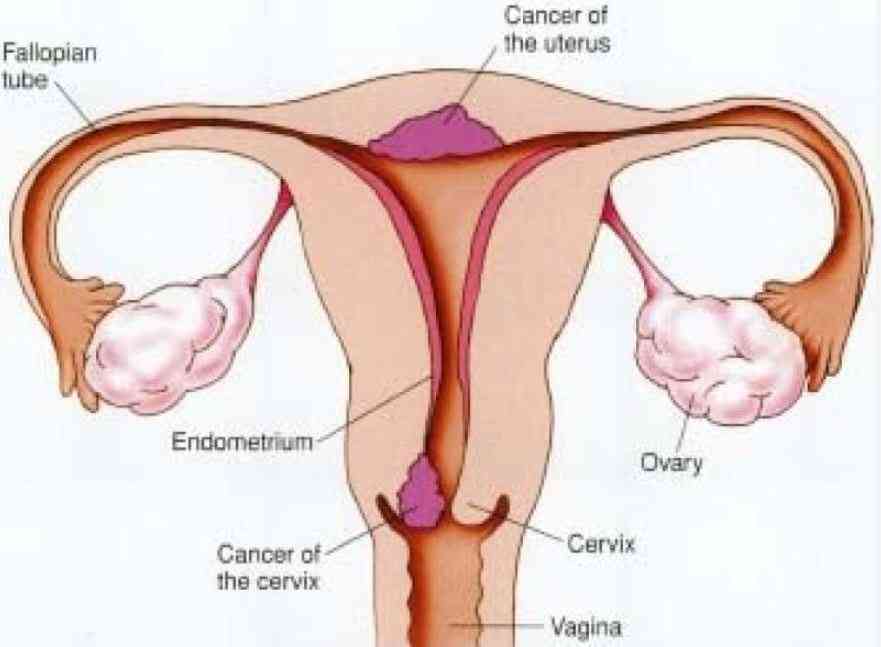
Among the tests was a pelvic ultrasound scan which showed that Julian’s reproductive tract was closed from the outside. This means that she didn’t have the vaginal opening but only the urethral opening and anus. Further tests also revealed that her uterus, ovaries and upper part of the vagina were missing. Doctors told her that she had a condition known as Mayer-Rokitansky-Küster-Hauser Syndrome (MRKH).
“I was shocked when I heard about this. I didn’t understand it fully yet but after a few days of brooding and bouts of crying, hoping it was a bad dream that would go away, I went back to my normal teen age life,” she recalls. Later, she would embark on a fact-finding mission, trying to understand what it was that plagued her body.
She would learn that MRKH was a condition that starts during foetal development and there is nothing her mother could have done to prevent it. That it was just her luck of the draw.
MRKH syndrome affects women only, and it is characterised by failure of the uterus and the vagina to develop either properly or at all.
Some women may however have normal ovarian function and normal external genitalia while for others, it doesn’t exist. Women with this disorder may develop normal secondary sexual characteristics such breast development and pubic hair, but not have a menstrual flow.
“I then understood that this could not be reversed and I had to live with it. It was a part of me,” Julian explains.
“My mum was shocked, my friends didn’t know about the condition until a few years ago when I went public about it.”
Some of Julian’s friends still think she is lying about it.
Failure to begin the menstrual cycle is the initial clinical sign of MRKH syndrome. About 1 in every 5,000 female babies have this condition.
Severity of the MRKH syndrome
The disorder can be broken down into two types, I and II. Type I syndrome is marked by the uterus and the vagina failing to develop properly. However the severity of MRKH syndrome type I may vary greatly from one person to another.
Type II occurs with additional anomalies that affect the kidneys preventing proper development as well as various skeletal malformations, mainly vertebral.
Renal abnormalities resulting from this disorder may cause growth deficiency, kidney stones, an increased susceptibility to urinary tract infections and abnormal accumulation of urine in the kidney due to obstruction.
Late diagnosis
Dr Felix Oindi, a consultant gynaecologist at Aga Khan University Hospital, says that most people only find out that they have the syndrome when they have reached puberty and their menses haven’t began.
“When we start determining the causes of the delay, then most of the time, we find that they don’t have a uterus, cervix and upper part of birth canal,” he says.
The lower part of the birth canal will however still be present.
What makes it difficult to tell when one has MRKH early is because other signs of puberty like breast development and growth of pubic hair are present.
“This is because, for most of the patients, the problem is not in the ovaries. They will be producing hormones normally,” Dr Oindi says.
Is normal sex life and motherhood achievable?
Many MRKH patients present with infertility or cannot have intercourse because the vagina is not well developed so full penetration is difficult.
“To help the patients have a near normal life, there is a surgery that can improve their sexual function and this is done by increasing the size of the vagina,” Oindi says.
Since she had no vaginal opening, Julian underwent a surgery in 2018 to create a vaginal canal. This would enable her to at least engage in intercourse; something she is still not ready for.
“When it comes to relationships, I have been open about my condition. Things haven’t worked out so far. I am aware that making the disclosure may often affect the future of my relations but I prefer to put it out there anyway,” she says.
She however hopes that one day, despite her condition, she will have a family of her own.
“I know I can’t have biological children because I don’t have ovaries either, so even IVF or surrogacy is out of question, but if God wills, I will adopt.”
Oindi says that uterine transplant is an option for the patients without a uterus.
“A few uterine transplants have actually been done and some of the women have gone ahead to get pregnant and safely deliver babies.
“This is however not a common procedure and Kenya is yet to do one,” he explains, adding that many patients will also require IVF after the transplant.
“In other cases, where women have their ovaries intact, they can become mothers through surrogacy. Their eggs can be harvested and a surrogate can carry the pregnancy to term for them.”
Experts estimate that about 20 per cent of women who present with no menses after reaching the age of puberty, will have MRKH. There is currently no data showing how common this condition is in Kenya.
“I choose to share my story to encourage fellow women going through a similar situation. I want them to understand that they are not alone in this.
“You only live once -- so be happy and love who you are. You can’t give what you don’t have,” Julian says.
 The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.
The Standard Group Plc is a multi-media organization with investments in media
platforms spanning newspaper print
operations, television, radio broadcasting, digital and online services. The
Standard Group is recognized as a
leading multi-media house in Kenya with a key influence in matters of national
and international interest.