×
The Standard e-Paper
Fearless, Trusted News
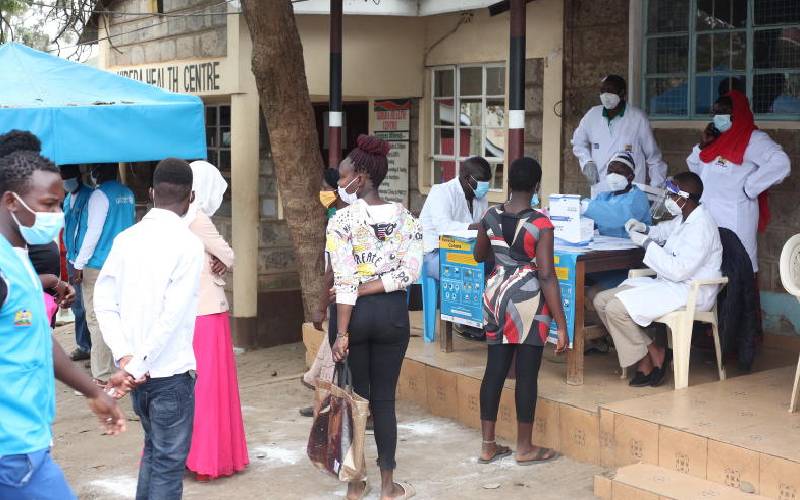
People queue for Covid-19 mass testing at the Kibra DO's Office in Nairobi. [Wilberforce Okwiri]
Medical insurers posted a 93.8 per cent drop in underwriting profits last year on increased healthcare claims as patients resumed hospital visits after overcoming fears of contracting Covid-19.






