×
The Standard e-Paper
Fearless, Trusted News
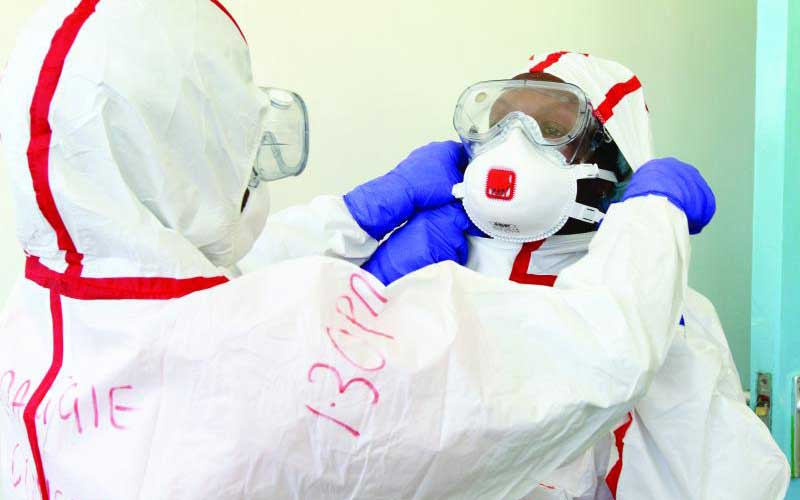
Health workers wear protective gear at Mbagathi Hospital, Nairobi. Kenya needs to strengthen its healthcare system to deal with pandemics such as Covid-19. [Elvis Ogina, Standard]
Inadequacy of healthcare infrastructure limits any progress towards attaining the third sustainable development goal (SDG) on good health and well-being.