×
The Standard e-Paper
Smart Minds Choose Us
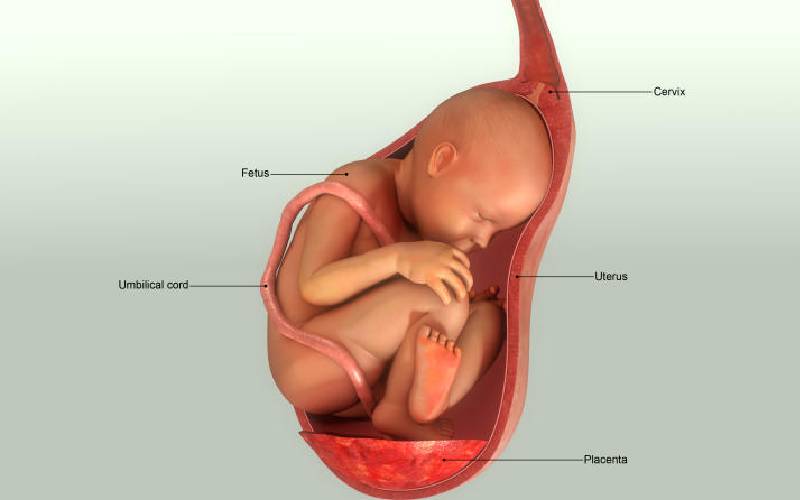
Immediately after birth, it was rather obvious to the doctors that something was wrong with baby Furaha. One side of the newborn’s body was slightly larger than the other- a condition known as hemihypertrophy. And she had an abnormally big head.