×
The Standard e-Paper
Join Thousands Daily
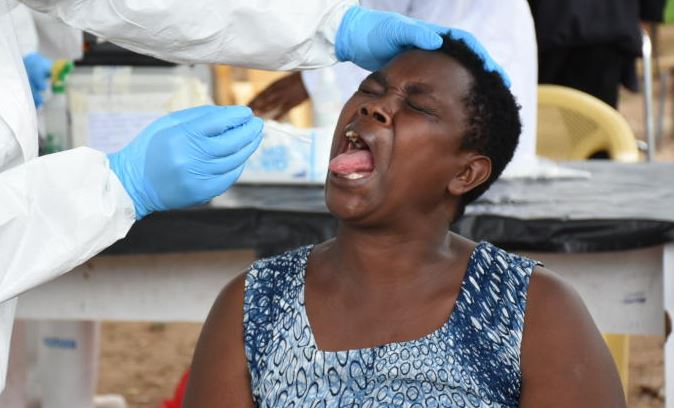
The Ministry of Health has fallen critically short of the estimated number of Covid-19 tests it hoped to have done by now.
Initially, officials from the ministry had said that by this time, some 66 days after the announcement of the first case, the country will have conducted close to 250,000, a number it ought to have hit by end of June.